Articles
- Page Path
- HOME > J Trauma Inj > Volume 37(1); 2024 > Article
-
Case Report
Atypical Vancouver B1 periprosthetic fracture of the proximal femur in the United Kingdom: a case report challenged by myeloma, osteoporosis, infection, and recurrent implant failures -
Sayantan Saha, Mch
 , Azeem Ahmed, FRCS
, Azeem Ahmed, FRCS , Rama Mohan, FRCS
, Rama Mohan, FRCS
-
Journal of Trauma and Injury 2024;37(1):89-96.
DOI: https://doi.org/10.20408/jti.2023.0069
Published online: March 18, 2024
- 355 Views
- 13 Download
Department of Trauma and Orthopaedics, North Manchester General Hospital, Manchester, UK
- Correspondence to: Sayantan Saha, Mch Department of Trauma and Orthopaedics, North Manchester General Hospital, Crumpsall, Manchester M8 5RB, UK Tel: +44-758-596-3270 Email: sayantan.saha@mft.nhs.uk
© 2024 The Korean Society of Traumatology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
- The indications for total hip replacement are increasing and not limited to osteoarthritis. Total hip replacement may also be done for trauma and pathological fractures in patients otherwise physiologically fit and active. This trend has led to an inevitable rise in complications such as periprosthetic femoral fracture. Periprosthetic femoral fracture can be challenging due to poor bone quality, osteoporosis, and stress fractures. We present a case of periprosthetic femoral fracture in a 71-year-old woman with some components of an atypical femoral fracture. The fracture was internally fixed but was subsequently complicated by infection, implant failure needing revision, and later stress fracture. She was on a bisphosphonate after her index total hip replacement surgery for an impending pathological left proximal femur fracture, and this may have caused the later stress fracture. Unfortunately, she then experienced implant breakage (nonunion), which was treated with a biplanar locking plate and bone grafting. The patient finally regained her premorbid mobility 13 months after the last surgery and progressed satisfactorily towards bony union.
- Periprosthetic femoral fractures (PFFs) are clinically challenging, especially in patients with comorbidities or other conditions that affect bone quality. With the significant rise in total hip replacement (THR) procedures over the past decade, clinicians can expect to encounter these challenges more often. According to data from the UK National Joint Registry [1], PFFs are the third most common cause of revision, and this value has nearly doubled in the past 8 years. The first consideration in the management of PFFs is assessing the stability of the prosthesis stem (Vancouver classification by Masri et al. [2]). The choice of fixation and the expected results depend on the extent of the bone stock and quality. In this case, the bone quality was worse than what was anticipated from the initial assessment and radiological pictures. In addition, there were features of an atypical femoral fracture (AFF) including a history of prolonged bisphosphonate usage, no associated trauma, prodromal symptoms, and a stress fracture line along the lateral cortex that later led to the transverse pattern of the PFF. This case was complicated by prolonged chemotherapy and steroid intake that created an immunocompromised state predisposing to risk of infection and may have led to the subsequent implant failure.
INTRODUCTION
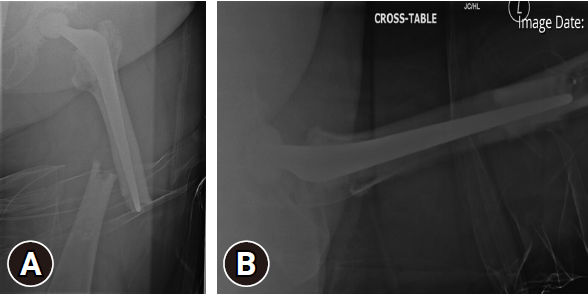
- A 71-year-old woman presented with pain in her left thigh and difficulty in weight-bearing following a history of jarring her left leg while getting up from a chair 6 weeks ago. A plain x-ray revealed a stress fracture just below the left long stem of a THR done 13 years ago (Fig. 1). On examination, she had some tenderness over the left thigh, but normal range of motion of the hip and no signs of infection. She was able to bear weight with a single cane.
- Her past medical history was significant for myeloma for which she had undergone two stem cell transplants and chemotherapy, including courses of high-dose steroids. She underwent bilateral THRs for myeloma deposits in both femurs, which were at risk of impending fractures. The left THR (cemented long stem) and right THR (cemented standard) were done at another facility 13 and 11 years ago, respectively. She had a right distal femur fracture (repaired with retrograde nailing) and a subsequent peri-implant fracture (treated with open reduction and internal fixation [ORIF] plating). She had been on bisphosphonate therapy for the past 8 years.
- Investigations
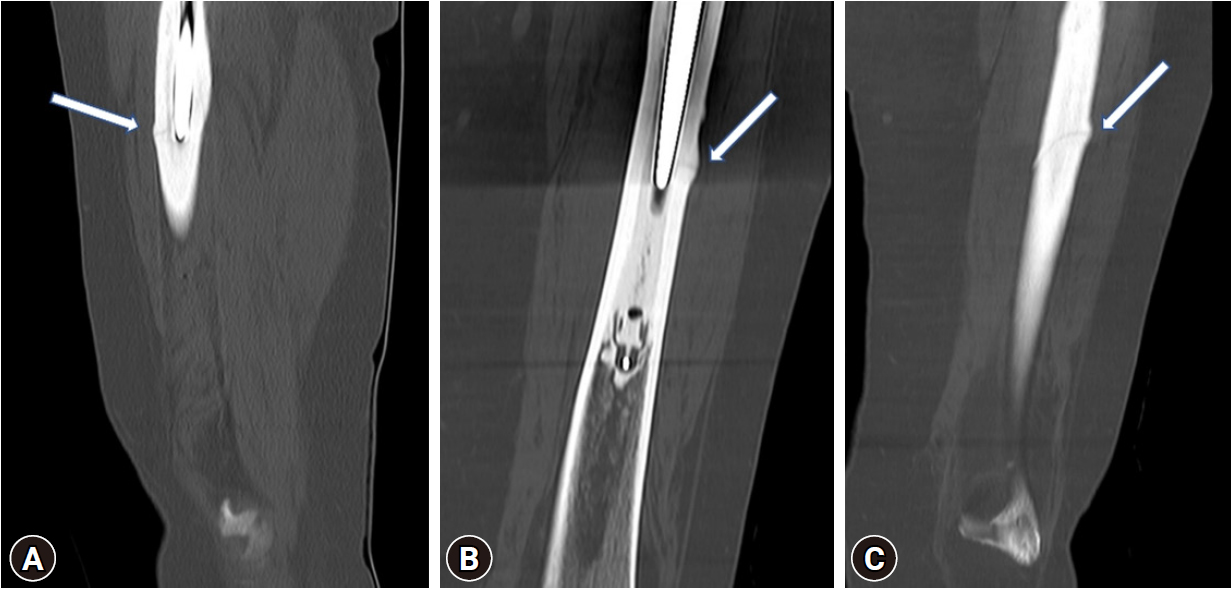
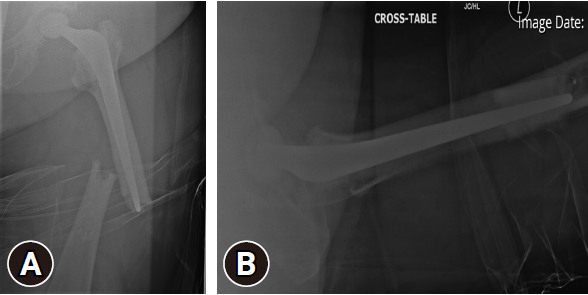
- The plain radiograph showed a fracture line of the lateral cortex with some stress reaction just distal to the tip of the stem, but the cement mantle and stem were intact and well fixed (Fig. 1). This was corroborated by a subsequent computed tomography (CT) scan of the left hip and femur (Fig. 2). Therefore, the decision was made to conservatively manage the fracture, and the patient was kept in protected weight-bearing. Unfortunately, she presented approximately 2 months later with a completely displaced fracture (transverse) in the same spot (Fig. 3).
- A CT scan was done showing stability of the prosthesis stem (Vancouver B1 fracture). The CT scan did not demonstrate any myeloma deposits in the femur (the disease was in remission), and a pathological cause was ruled out after discussion with the haemato-oncologist.
- Blood investigations were within normal limits (10×109/L), and the C-reactive protein (CRP) level was not elevated (15 mg/L), ruling out infection. The immediate postoperative blood markers were also unremarkable. Operative notes from the previous surgery (primary THR) were accessed for details of the implants used and the surgical approach employed.
- Treatment
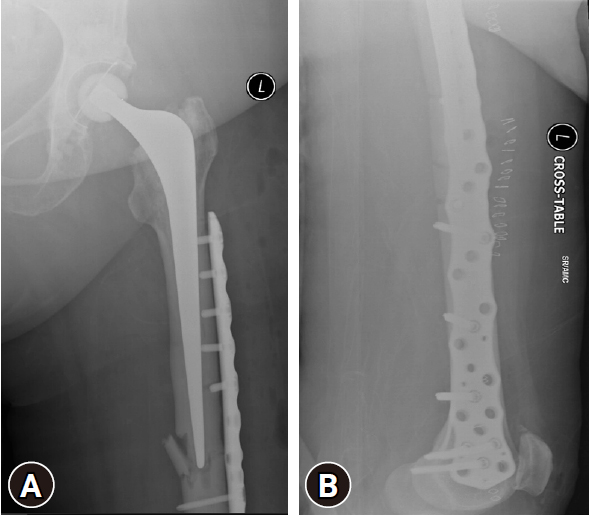
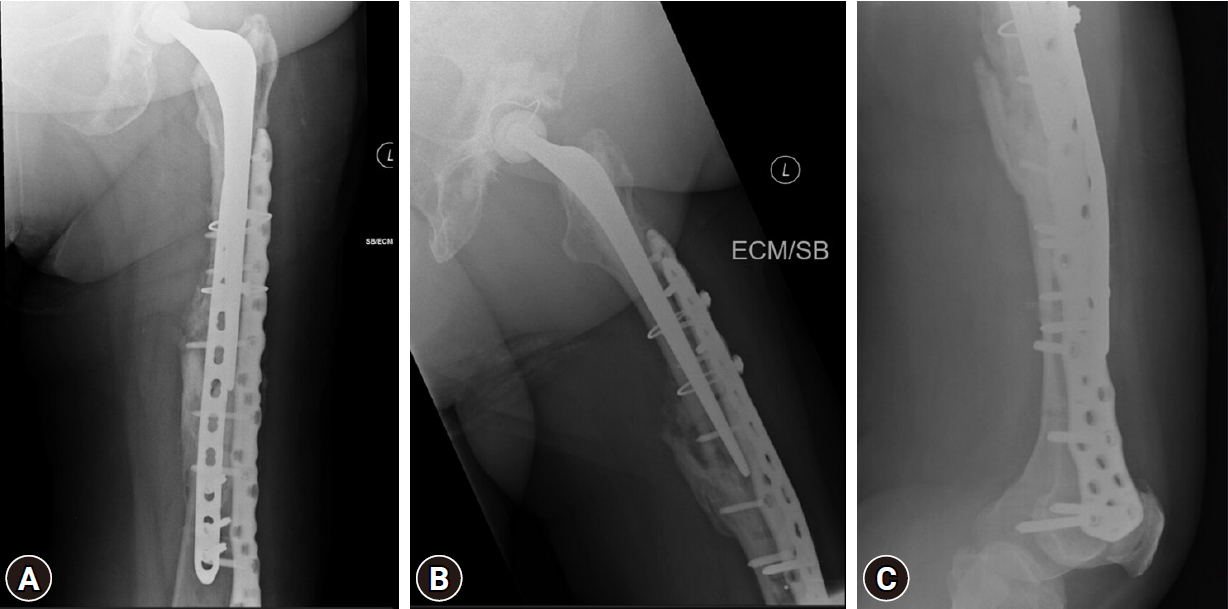
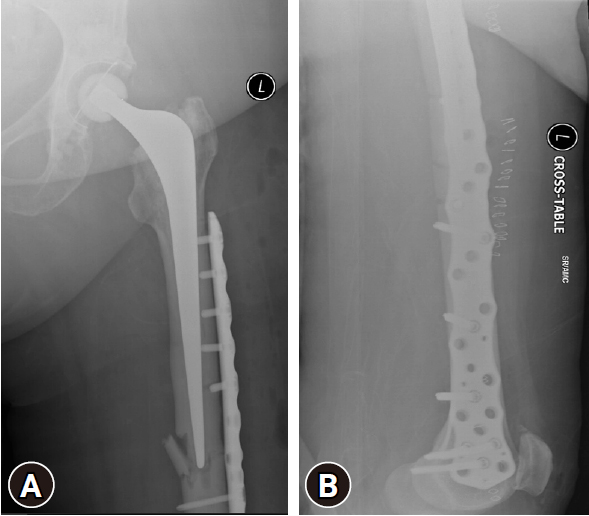
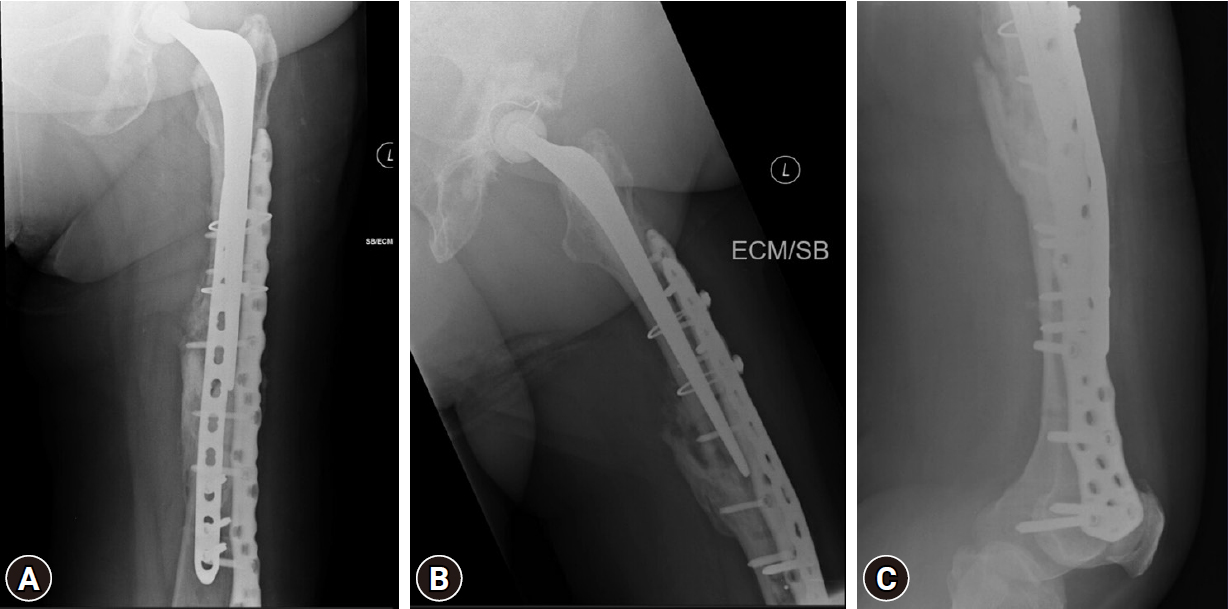
- The fracture was anatomically reduced and fixed with a long Non-Contact Bridging (NCB) periprosthetic plate (Zimmer Biomet Institute) after ensuring that the stem and the cement mantle were stable. Bone grafting was done (allograft) due to poor bone quality (Fig. 4). The decision was made to use a long plate that spanned to the distal femur to avoid a stress riser distally and avoid complications later.
- Unfortunately, she presented within a month with infection (white cells, 15×109/L; CRP, 79 mg/L) and failed fixation. She was started on broad-spectrum antibiotics (co-amoxiclav with teicoplanin), and the implant was removed. Her antibiotics were changed to levofloxacin and rifampicin (as per culture and sensitivity reports from the intraoperative infected tissue sample). After a week, she was taken for a second debridement under the cover of antibiotics. Intraoperatively, the fracture site was found to be relatively clean, free of pus and unhealthy tissue, and the inflammatory markers were trending down (white cells, 11×109/L; CRP, 46 mg/L). Therefore, it was decided to proceed with ORIF in the same sitting using the NCB plate and cerclage wire. Her postoperative period was unremarkable, and she was discharged on oral antibiotics for 10 weeks. Subsequent clinical follow-up examinations showed good progress, with her CRP slowly coming down. A 6-month postoperative x-ray showed satisfactory callus, though radiological union was still not complete (Fig. 5). Clinically, she was weight-bearing without any pain using a single stick.
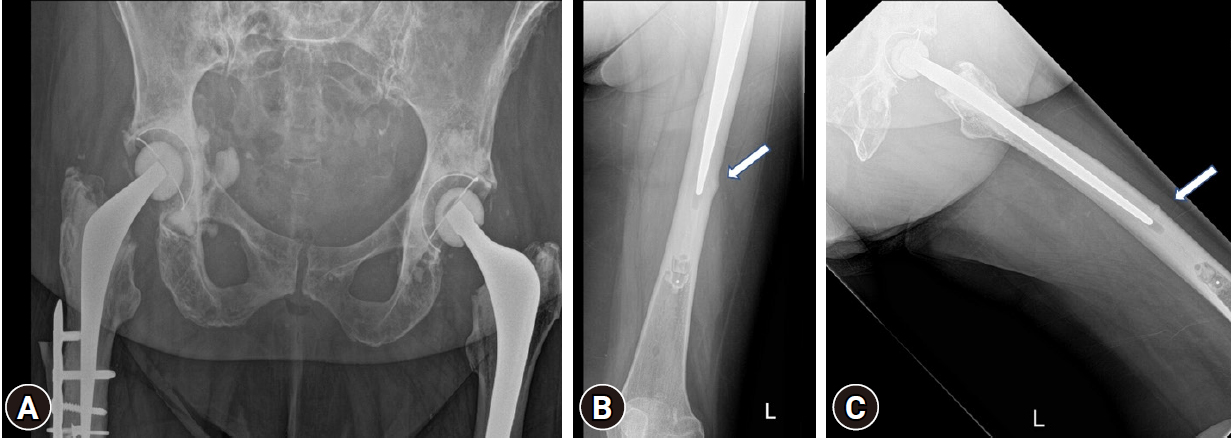
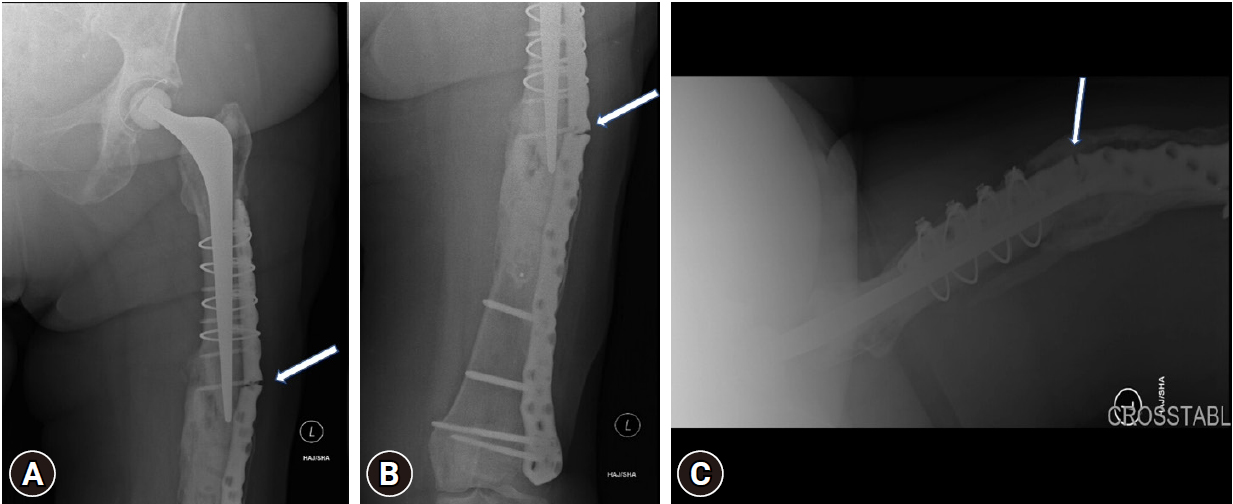
- After a year, she presented again with progressive pain in the left thigh and difficulty weight-bearing for the past 10 weeks. Again, there was no history of trauma (the delay in presentation and gap in follow-up were due to COVID-19 pandemic restrictions). The x-ray revealed a break in the plate near the fracture site with some varus collapse (Fig. 6). Although, radiologically, there was no new fracture or significant displacement, and some bridging callus was present, the fracture was not united. This was confirmed with CT. However, the THR prosthesis stem was still stable and there were no signs of loosening, so revision arthroplasty was avoided.
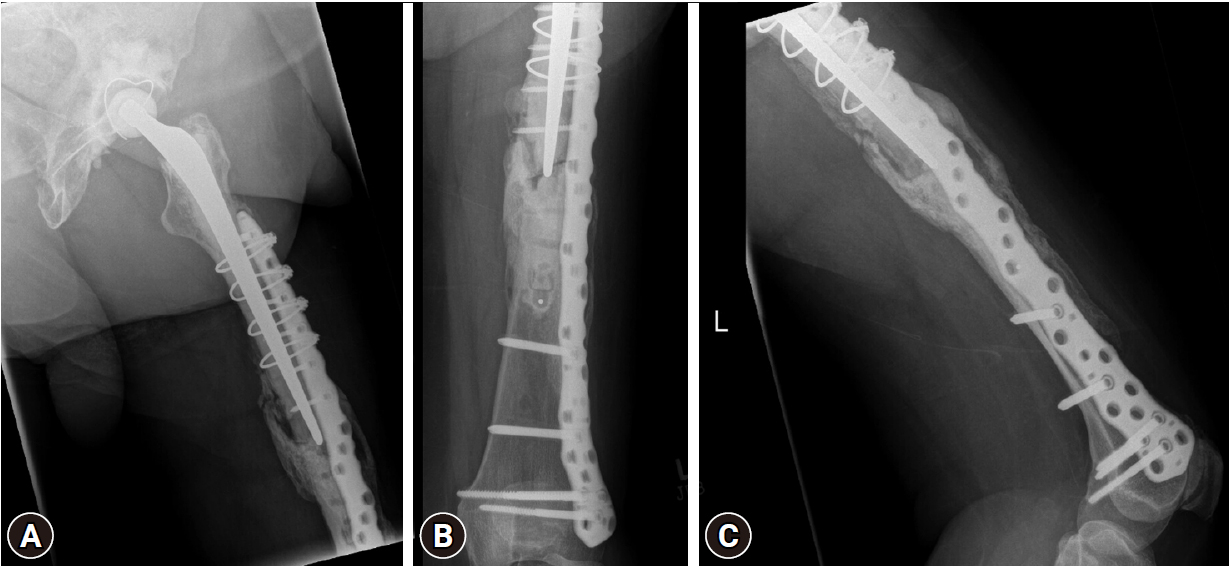
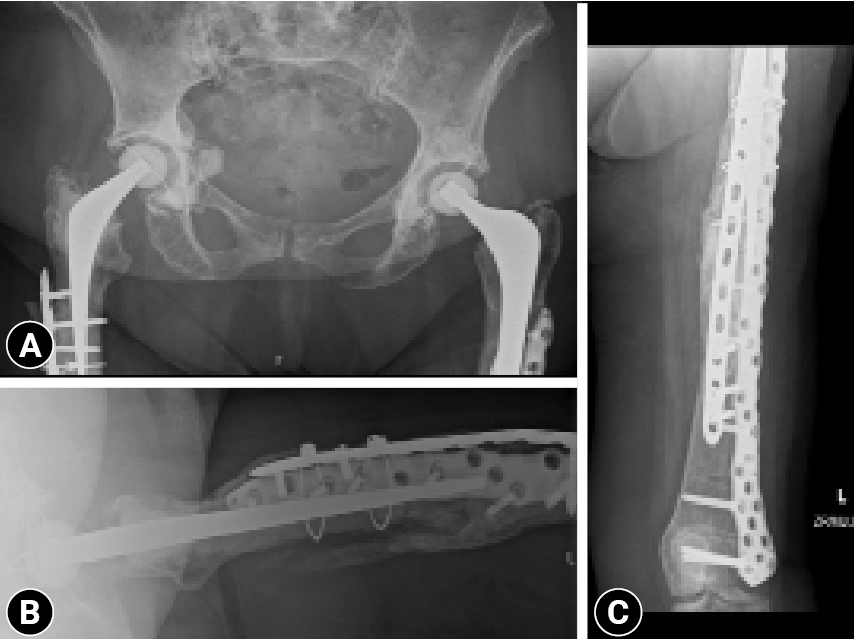
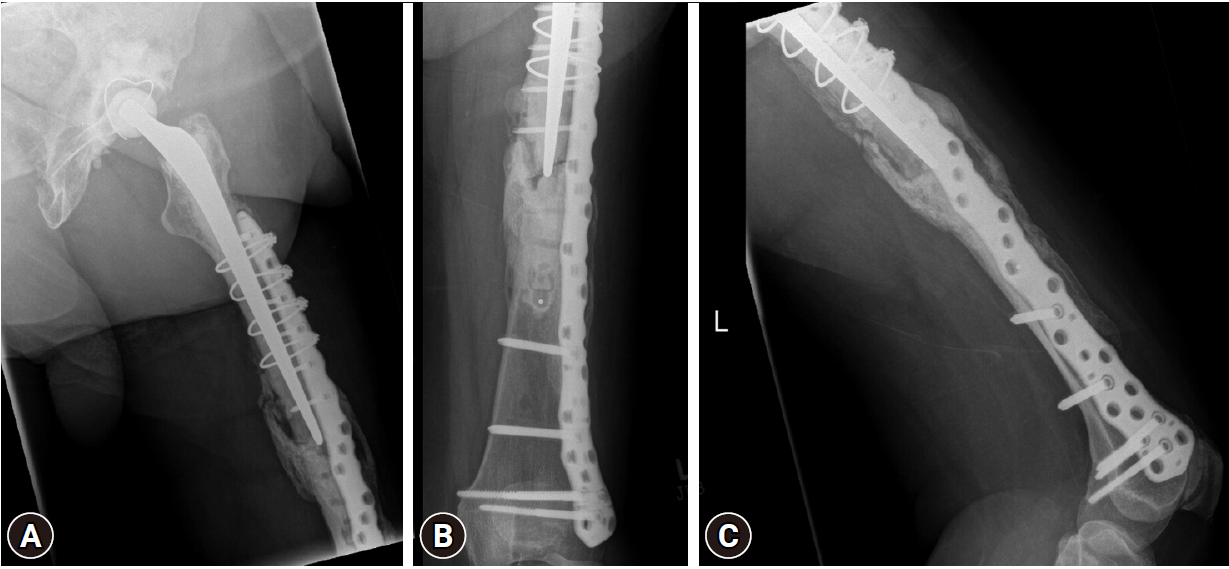
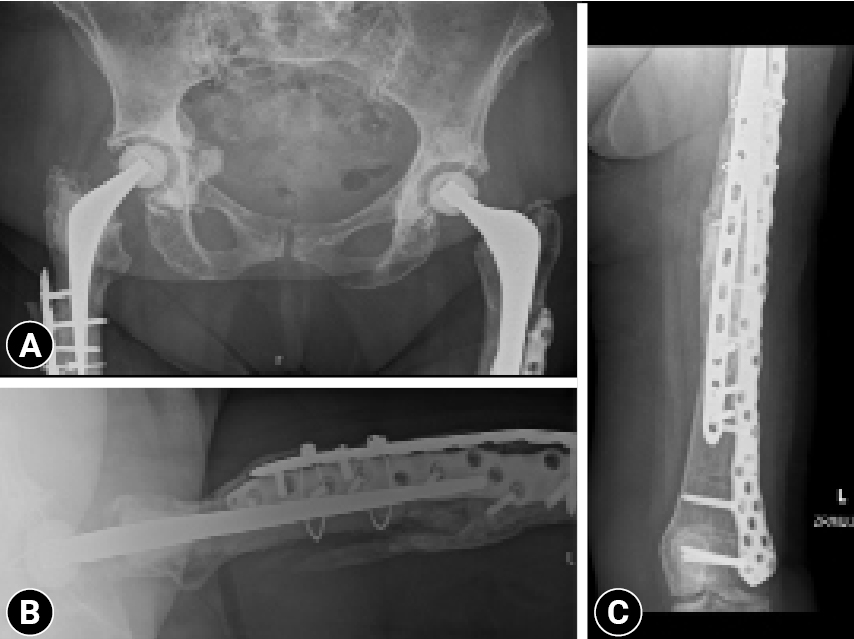
- She underwent surgery once again. The broken plate was removed, the fracture edges were liberally freshened, and then dual plating (anterior locking compression plate and lateral NCB plate) with bone grafting (allograft) was done. The postoperative period was uneventful, and after a period of protected weight-bearing (6 weeks) she gradually restarted weight-bearing. At her 3-month follow-up she was able to fully weight bear painlessly. The X-ray was also reassuring, with a good bridging callus (Fig. 7).
- Outcome and follow-up
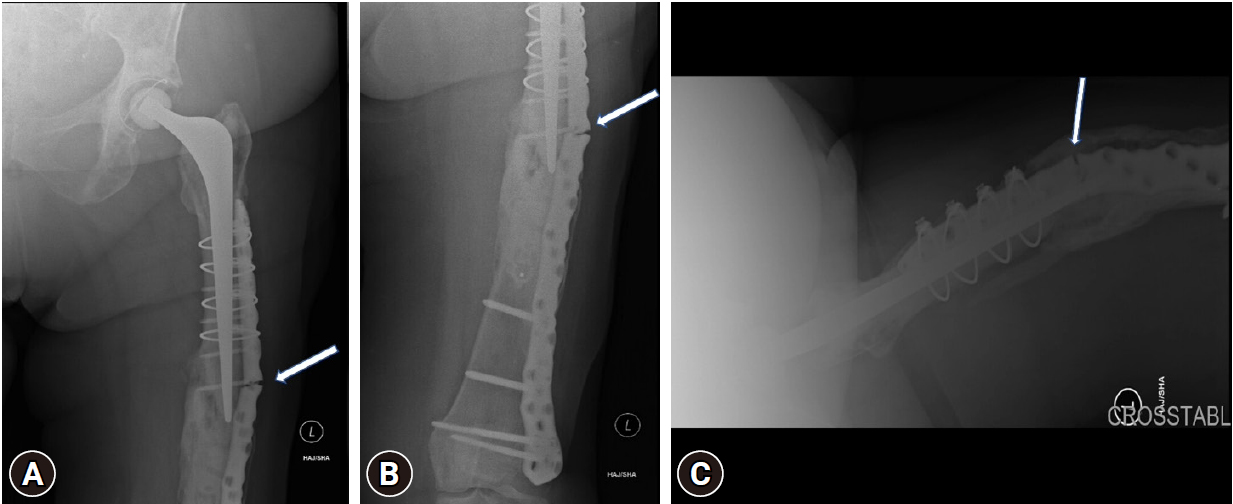
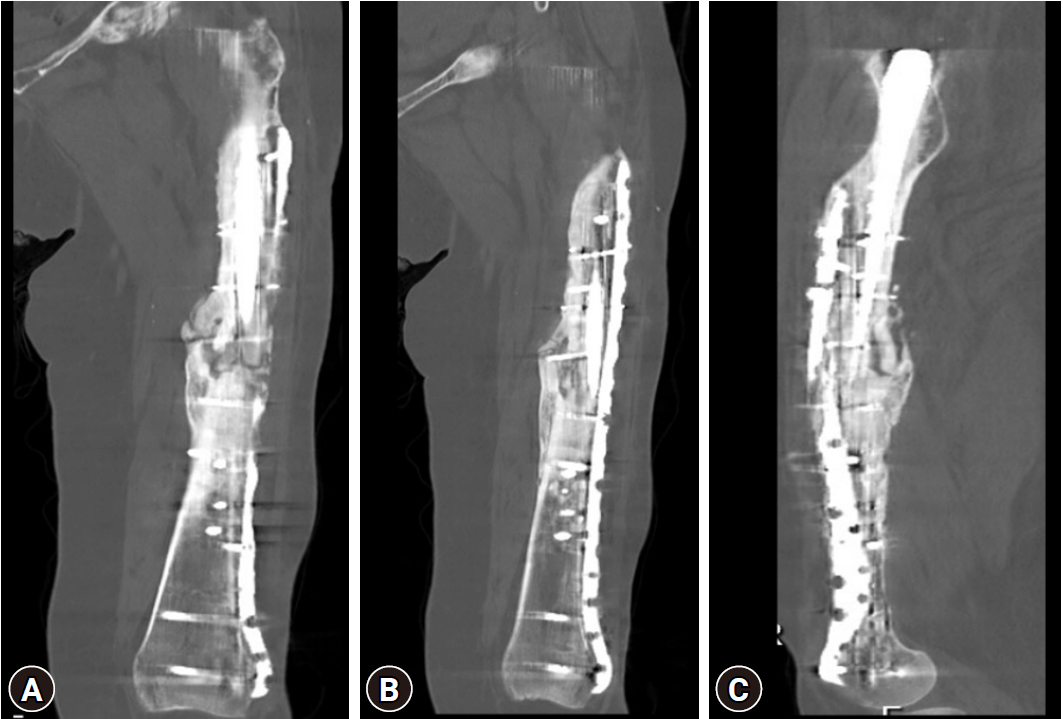
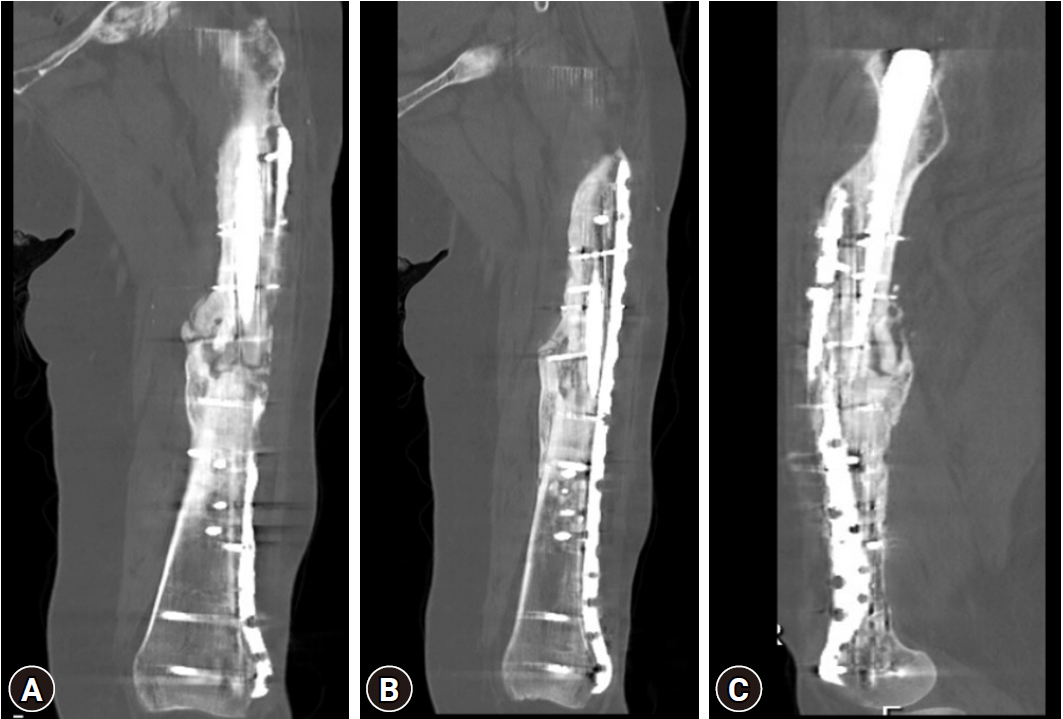
- At the 10-month follow-up, a fracture line was still visible in the posteromedial cortex, but clinically there were no concerns. A CT scan to assess the fracture union showed satisfactory callus and no implant loosening but highlighted the delayed union in two cortices (Fig. 8). To speed up the union, she was started on low-intensity pulsed ultrasound therapy (Exogen, Bioventus LLC). Her latest x-ray (2 months after starting Exogen therapy) showed better bridging callus and fracture consolidation (Fig. 9). At 13 months after the final surgery, she remained pain-free and had regained her premorbid mobility.
- Ethics statement
- This study was done in compliance with the principles of the Declaration of Helsinki. The study’s protocol was reviewed and approved by the Institutional Review Board of the NHS Trust (No. 2022-146). Written informed consent for publication and clinical images was obtained from the patient.
CASE REPORT
- Periprosthetic fractures significantly impact not only the patient, but also the healthcare system clinically and financially. The median cost of treating 75 PFFs in a UK tertiary referral center was £13,381 (ranging from £1,006–£53,763) with an overall loss of £373,737 over 2 years [3]. Therefore, it is imperative that equal focus be given to the prevention of these complex fractures as is given to their management. Though the American Society for Bone and Mineral Research (ASBMR) excludes PFFs from the definition of AFF [4,5], several cases of PFF have been reported with atypical features fitting the definition of AFF [6,7]. Studies comparing typical AFFs and isolated AFFs with periprosthetic AFFs have highlighted a longer time of union in the periprosthetic AFFs, as well as higher rates of reoperation and infection [8,9]. Apart from mechanical factors (e.g., lateral femoral bow in the frontal plane, poor bone stock), biological factors play an important role in the causation of these atypical fractures. Bisphosphonates suppress bone turnover, and in the process interfere with bone remodeling and the healing of microfractures and stress fractures [10,11].
- In this case, the initial fixation was anatomical, engaging eight cortices on either side of the fracture and spanning to the distal femur to avoid the risk of stress risers. The fixation failed due to infection and not to lack of stability. The patient’s background myeloma with a history of chemotherapy and long-term steroid treatment could explain the immunocompromised state that led to the failure. This was clinically anticipated but unavoidable in practice and could not be attributed to surgical lacunae. A staged revision was done under antibiotic coverage with a similar length NCB plate, bone grafting, and cerclage wiring. Bone grafting was considered because the medial cortex was found to have significant bone loss from infection and subsequent debridement. For similar reasons, cerclage cable fixation was also done to provide additional stability. The prosthesis was not revised as the stem was already long and was found to be stable on both preoperative CT scan and intraoperative clinical assessment. The patient was kept on prolonged antibiotic therapy and reinfection was successfully averted. Unfortunately, however, the fracture went into delayed nonunion (varus collapse) ultimately leading to plate breakage 1 year after the surgery. Retrospectively, the reason for failure could be attributed to poor bone quality, bone loss and lack of medial cortical support (despite bone grafting), and the likely inadequate stability provided by the single internal fixation. In addition, infection might have led to scarred granulation tissue that failed to neovascularize and thus failed to form adequate callus. Therefore, in the last surgery, the nonunion fracture ends were liberally freshened (including removal of all scarred tissue), anatomical reduction was achieved, and then internally fixed with biplanar plates (anterior and lateral). The fracture gaps were generously packed with bone grafts. Fixation in two planes increased rotational stability by allowing the placement of multidirectional locking screws and utilizing all the staggered screw holes in the polyaxial locking NCB plate system [11]. Usually, in PFFs and AFFs, lateral plating suffices, as this contributes to adequate stability at the fracture site and acts to some extent as tension band plating [12]. However, in our case this was not adequate for multiple reasons, including infection, poor native bone stock, myeloma, the atypical nature of the fracture, and metabolic bone disease. Though biplanar plating may be considered overkill for regular PFFs, the usage was justified in this scenario.
- Arguments may be made in this case against internal fixation and to consider this unstable fracture pattern (atypical and transverse) as B2 and not B1, despite having a stable stem. In that scenario, the ideal treatment would have been revision of the stem. However, the treatment decision in our case (dual plating) was based on the patient already having a long stem in situ that was clearly stable with an intact cement mantle per the preoperative and intraoperative assessments of two different hip revision surgeons. In addition, stem revision in this complex case with a difficult medical background would have unnecessarily prolonged the operating time and increased the risk of infection. The option of biplanar locking plates has been supported in similar cases by Chakrabarti et al. [11] and the Swedish registry-based cohort study by Chatziagorou et al. [13].
- Considering the difficulties and challenges faced in this case, as well as the multidisciplinary involvement in treatment, it serves as an ideal example of what to expect when managing PFFs with atypical features and complications. This case highlights the significance of a detailed history, the importance of preoperative planning with a clinical and radiological workup, and a stepwise approach to complications.
DISCUSSION
-
Author contributions
Conceptualization: SS, AA; Formal analysis: SS, RM; Methodology: SS, RM; Visualization: SS; Writing–original draft: SS; Writing–review & editing: all authors. All authors have read and approved the final manuscript.
-
Conflicts of interest
The authors have no conflicts of interest to declare.
-
Funding
The authors received no financial support for this study.
-
Data availability
Data sharing is not applicable as no new data were created or analyzed in this study.
ARTICLE INFORMATION
- 1. NJR Reports. Hips: revision procedures: patient characteristics [Internet]. UK National Joint Registry; 2021 [cited 2021 Sep 18]. Available from: https://reports.njrcentre.org.uk/hips-revision-procedures-patient-characteristics.
- 2. Masri BA, Meek RM, Duncan CP. Periprosthetic fractures evaluation and treatment. Clin Orthop Relat Res 2004;(420):80–95. Article
- 3. Ramavath A, Lamb JN, Palan J, Pandit HG, Jain S. Postoperative periprosthetic femoral fracture around total hip replacements: current concepts and clinical outcomes. EFORT Open Rev 2020;5:558–67.
- 4. Shane E, Burr D, Ebeling PR, et al. Atypical subtrochanteric and diaphyseal femoral fractures: report of a task force of the American Society for Bone and Mineral Research. J Bone Miner Res 2010;25:2267–94. PubMed
- 5. Shane E, Burr D, Abrahamsen B, et al. Atypical subtrochanteric and diaphyseal femoral fractures: second report of a task force of the American Society for Bone and Mineral Research. J Bone Miner Res 2014;29:1–23. PubMed
- 6. Chen F, Bhattacharyya T. Periprosthetic fracture of the femur after long-term bisphosphonate use: a case report. JBJS Case Connect 2012;2:e21. PubMed
- 7. Schaeffer JF, Attarian DE, Wellman SS. Periprosthetic femoral insufficiency fracture in a patient on long-term bisphosphonate therapy. The Duke Orthop J 2012;2:66–9. Article
- 8. Robinson Jde D, Leighton RK, Trask K, Bogdan Y, Tornetta P 3rd. Periprosthetic atypical femoral fractures in patients on long-term bisphosphonates: a multicenter retrospective review. J Orthop Trauma 2016;30:170–6. PubMed
- 9. Corten K, Vanrykel F, Bellemans J, Frederix PR, Simon JP, Broos PL. An algorithm for the surgical treatment of periprosthetic fractures of the femur around a well-fixed femoral component. J Bone Joint Surg Br 2009;91:1424–30. ArticlePubMedPDF
- 10. Pavlou G, Panteliadis P, Macdonald D, et al. A review of 202 periprosthetic fractures: stem revision and allograft improves outcome for type B fractures. Hip Int 2011;21:21–9. ArticlePubMedPDF
- 11. Chakrabarti D, Thokur N, Ajnin S. Cable plate fixation for Vancouver type-B1 periprosthetic femoral fractures: our experience and identification of a subset at risk of non-union. Injury 2019;50:2301–5. ArticlePubMed
- 12. Kharazmi M, Michaelsson K, Hallberg P, Schilcher J. Lateral fixation: an alternative surgical approach in the prevention of complete atypical femoral fractures. Eur J Orthop Surg Traumatol 2018;28:299–304. ArticlePubMedPMCPDF
- 13. Chatziagorou G, Lindahl H, Karrholm J. Surgical treatment of Vancouver type B periprosthetic femoral fractures: patient characteristics and outcomes of 1381 fractures treated in Sweden between 2001 and 2011. Bone Joint J 2019;101-B:1447–58. PubMed
REFERENCES
Figure & Data
References
Citations

 KST
KST

 PubReader
PubReader ePub Link
ePub Link Cite
Cite