Articles
- Page Path
- HOME > J Trauma Inj > Volume 35(2); 2022 > Article
-
Case Report
A case report of “minor” trauma leading to a major disability: whiplash-associated dysphagia, dysphonia, and dysgeusia -
Ami Schattner, MD1
 , Yair Glick, MD2
, Yair Glick, MD2
-
Journal of Trauma and Injury 2022;35(2):115-117.
DOI: https://doi.org/10.20408/jti.2021.0043
Published online: May 19, 2022
- 2,397 Views
- 33 Download
1The Faculty of Medicine, Hebrew University and Hadassah Medical School, Jerusalem, Israel
2Department of Imaging, Sanz Medical Centre, Ariel University, Netanya, Israel
- Correspondence to Ami Schattner, MD The Faculty of Medicine, Hebrew University and Hadassah Medical School, Sderot Churchill 8, Jerusalem 91240, Israel Tel: +972-8-939-0330 E-mail: amischatt@gmail.com
Copyright © 2022 The Korean Society of Traumatology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
- “Whiplash”-type injuries are commonly encountered and often cause neck pain, neck stiffness, and headaches. However, these injuries can have rare and poorly recognized complications, such as the development of a prevertebral hematoma leading to acute respiratory failure in the emergency department, followed by severe, life-threatening dysphagia and recurrent aspirations. In the patient described herein, a whiplash injury was accompanied by vocal cord paralysis and dysphonia (vagus nerve), dysgeusia (glossopharyngeal nerve, vagus nerve), and upper esophageal spasm (cricopharyngeal muscle, vagus nerve). It is unlikely that this was a complication of cervical fusion surgery. Instead, a combined stretch-induced lower cranial nerve injury, possibly on the exit of these nerves through the jugular foramen, seems to be a likely, but underappreciated mechanism occurring in rare instances of whiplash injuries.
- Blunt impact in motor vehicle collisions is not infrequently associated with sudden acceleration and deceleration, causing rapid extension of the head and neck followed by flexion [1]. These “whiplash” injuries often cause neck pain, neck stiffness, and headaches. However, prevertebral hematoma development and marked dysphagia are rare and poorly recognized complications [2].
INTRODUCTION
- An 80-year-old engineer driving home from work was hit by a bus from behind, and his vehicle collided with a fence. He had been on rivaroxaban and bisoprolol for paroxysmal atrial fibrillation. In the emergency department, he was alert and stable, and he complained of right neck pain where a hematoma was noted.
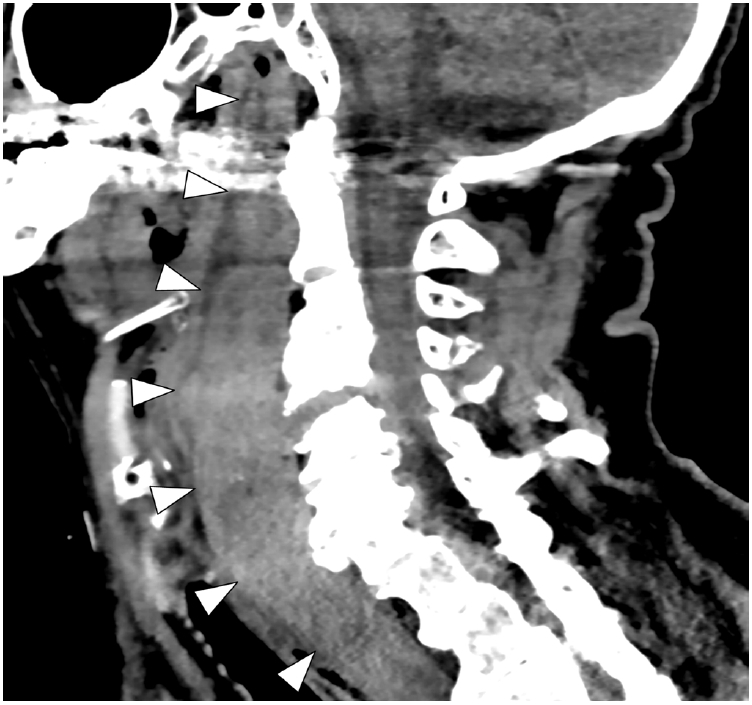
- Head and chest computed tomography (CT) were normal. Neck CT revealed a cervical prevertebral hematoma and fractured posterior tubercle of C4 (Fig. 1). The spinal cord showed no changes, as was also the case on subsequent magnetic resonance imaging, and the neurological examination was normal. Sudden respiratory failure mandated intubation, which was difficult to perform. He was given prothrombin complex concentrate to reverse rivaroxaban and underwent surgery on the next day with cervical fusion (C2–C7, posterior approach) and later, dexamethasone. After 2 weeks, it was deemed necessary to perform discectomy and fusion (C4–C5, anterior approach). After 3 weeks of intensive care due to recurrent pneumonia, the patient was extubated and started feeding. However, dysphagia with both solid and liquid foods appeared and persisted, associated with coughing, regurgitation, dysphonia, and dysgeusia causing dehydration, progressive distress, depression, and malnutrition (58 kg at 1 year vs. 71 kg prior; albumin, 1.8 g/dL vs. 3.8 g/dL) associated with extreme lassitude and marked functional decline and dependence. Dysphagia was suspected 3 weeks after the nasogastric tube was removed, but the full investigations took several months to obtain. The swallowing examinations were performed at an outpatient clinic specializing in swallowing disorders and were done 5 to 6 months after discharge. The investigations confirmed oropharyngeal dysphagia with normal tongue and lip function, a normal gag reflex, no dysarthria, or focal pyramidal signs, but hoarseness and right vocal cord paralysis on laryngoscopy. Fiberoptic endoscopic examination of swallowing (FEES) demonstrated food pooling in the valleculae, regurgitation, and liquid penetration triggering coughing. A videofluoroscopic evaluation with liquid barium and wet bread confirmed the FEES findings and also revealed failed relaxation of the upper esophageal sphincter with a normal esophageal phase. Eventually, after various oral intake manipulations failed, a nasogastric tube was inserted. When weight loss and hypalbuminemia persisted, parenteral nutrition through a peripherally inserted central catheter was instituted. The patient died of pneumonia 16 months after the accident.
CASE REPORT
- Dysphagia, a subjective sensation of difficulty of swallowing with or without pain (odynophagia), signifies an abnormality in the passage of solid food and/or liquids from the oral cavity to the stomach. Practically, oropharyngeal versus esophageal dysphagia can be distinguished, and each subset has multiple etiologies. When evaluating dysphagia, good history-taking can often direct the clinician to the underlying cause. For example, oropharyngeal dysphagia is frequently characterized by difficulty in initiating swallowing, feeling of food sticking in the throat and associated “early” coughing and choking, often with pharyngeal complaints (nasal regurgitation, sialorrhea, changed voice) and recurrent aspiration pneumonia [3,4].
- Our patient’s isolated neck trauma seemed minor at first, but there is no doubt that his anticoagulant treatment contributed to the growth of the hematoma, airway compression, and acute respiratory failure (Fig. 1) [2]. Other notable features included persistent oropharyngeal dysphagia (as described above) causing progressive malnutrition, weight loss, hypalbuminemia, and aspiration pneumonia, ultimately leading to his demise. This occurred with only a minor fracture and no demonstrable neurological deficit or cord involvement on neuroimaging.
- Unlike cervical osteoarticular disease, which is an acknowledged although uncommon cause of oropharyngeal dysphagia, whiplash-associated cranial nerve injury and anatomical changes of the oropharynx with dysphagia have been rarely reported [5,6]. In view of the patient’s associated vocal cord paralysis and dysphonia (vagus nerve), dysgeusia (glossopharyngeal nerve, vagus nerve), and upper esophageal sphincter spasm (cricopharyngeal muscle innervated by the vagus), a combined stretch-induced lower cranial nerve injury, possibly on the exit of these nerves through the jugular foramen, seems likely. Patients may develop dysphagia after cervical surgery, but unlike our patient, their dysphagia is isolated and usually improves over 6 months; severe dysphagia is rare (e.g., 6 of 186 patients, 3.2%) [7]. Thus, physicians in the emergency department and varied disciplines need to be aware of the unusual but highly disabling association of misleadingly “simple” whiplash injury with acute respiratory failure and subsequent significant impairment of swallowing, phonation, and taste.
DISCUSSION
-
Ethical statements
Informed consent for publication of the research details and clinical images was obtained from the patient’s next of kin.
-
Conflicts of interest
The authors have no conflicts of interest to declare.
-
Funding
None.
-
Author contributions
Conceptualization: AS; Data curation: all authors; Formal analysis: AS; Writing–original draft: AS; Writing–review & editing: all authors.
All authors read and approved the final manuscript.
ARTICLE INFORMATION
- 1. Schofferman J, Bogduk N, Slosar P. Chronic whiplash and whiplash-associated disorders: an evidence-based approach. J Am Acad Orthop Surg 2007;15:596–606. ArticlePubMed
- 2. Anagnostara A, Athanassopoulou A, Kailidou E, Markatos A, Eystathidis A, Papageorgiou S. Traumatic retropharyngeal hematoma and prevertebral edema induced by whiplash injury. Emerg Radiol 2005;11:145–9. ArticlePubMed
- 3. Scharitzer M, Pokieser P, Wagner-Menghin M, Otto F, Ekberg O. Taking the history in patients with swallowing disorders: an international multidisciplinary survey. Abdom Radiol (NY) 2017;42:786–93. ArticlePubMed
- 4. Spieker MR. Evaluating dysphagia. Am Fam Physician 2000;61:3639–48. PubMed
- 5. Helliwell M, Robertson JC, Todd GB, Lobb M. Bilateral vocal cord paralysis due to whiplash injury. Br Med J (Clin Res Ed) 1984;288:1876–7. Article
- 6. Stone D, Bogaardt H, Linnstaedt SD, et al. Whiplash-associated dysphagia: considerations of potential incidence and mechanisms. Dysphagia 2020;35:403–13. ArticlePubMed
- 7. Zeng JH, Zhong ZM, Chen JT. Early dysphagia complicating anterior cervical spine surgery: incidence and risk factors. Arch Orthop Trauma Surg 2013;133:1067–71. ArticlePubMed
REFERENCES
Figure & Data
References
Citations

 KST
KST

 PubReader
PubReader ePub Link
ePub Link Cite
Cite


