Articles
- Page Path
- HOME > J Trauma Inj > Volume 34(1); 2021 > Article
-
Case Report
Surgically Removed Intrapulmonary Shotgun Pellet without Traumatic Hemopneumothorax - Soo Young Yoon, M.D.1, Young Hoon Sul, M.D., Ph.D.2,3
-
Journal of Trauma and Injury 2021;34(1):66-69.
DOI: https://doi.org/10.20408/jti.2020.0026
Published online: March 23, 2021
- 3,140 Views
- 92 Download
1Department of Thoracic and Cardiovascular Surgery, Chungbuk National University Hospital, Cheongju, Korea
2Department of Trauma Surgery, Chungbuk National University Hospital, Cheongju, Korea
3Department of Trauma Surgery, College of Medicine, Chungbuk National University, Cheongju, Korea
- Correspondence to Young Hoon Sul, M.D., Ph.D. Department of Trauma Surgery, Chungbuk National University Hospital, 776 1sunhwan-ro, Seowon-gu, Cheongju 28644, Korea Tel: +82-43-269-7847 Fax: +82-43-269-7810 E-mail: ssulyh@gmail.com
• Received: July 20, 2020 • Revised: September 17, 2020 • Accepted: October 12, 2020
Copyright © 2021 The Korean Society of Traumatology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
- When treating firearms injuries, knowledge of the proper management is important because these injuries have high morbidity and mortality. However, due to strict gun safety regulations, surgeons in Asia often have limited experiences with gunshot wound management. Recently, the authors had the experience of removing a bullet that did not cause hemopneumothorax, but remained in the lung parenchyma. Due to the risk of complications that could occur if the bullet was not removed, surgical treatment was eventually performed to remove the bullet. A literature review was needed to determine whether this treatment was appropriate. We concluded that removing the bullet could prevent incidental complications. In this regard, the authors report a case along with a review of the relevant literature to suggest appropriate treatment directions for surgeons who do not have experience with gunshot wounds.
- In the United States, where guns are freely available, chest penetration injuries, including gunshot wounds (GSWs), are common enough to account for about 7% of all trauma, but these injuries are relatively rare in Asian countries where firearms are tightly regulated [1]. Thoracic GSWs have a high mortality rate from damage to major organs, such as the heart or lungs, and should be treated promptly and carefully. However, although there is evidence of long-term damage from chest wounds and bullets remaining in the rib cage, conservative treatment should be prioritized without bullet removal in stable patients. However, in rare cases, complications due to foreign body reactions have been reported, and disagreements over whether or not this treatment policy is appropriate can lead to a dilemma for the medical staff who need to determine the direction of treatment [2-5]. The authors report an experience of treating a patient with a metal pellet in the lung parenchyma due to a recent shotgun injury, but without hemothorax or pneumothorax, and review the literature regarding the appropriate treatment plan for such cases.
INTRODUCTION
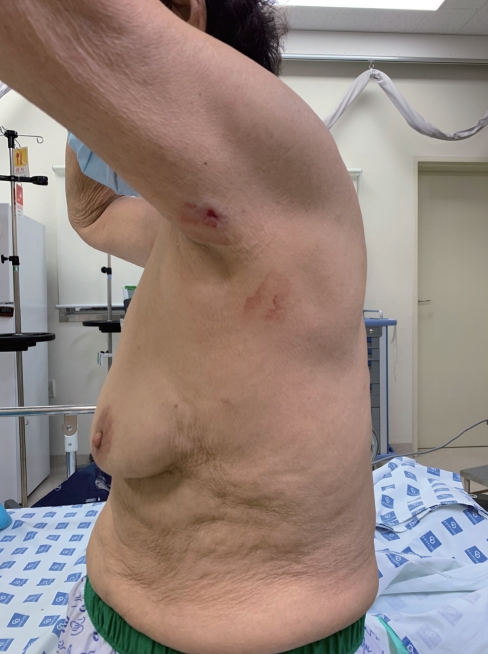
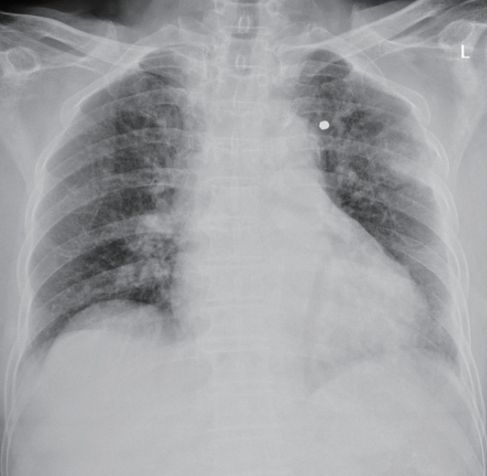
- An 80-year-old woman walked into the emergency room with a small amount of hemoptysis and mild dyspnea combined with sudden left axillary pain after being injured by a gunshot while working in the field. Her vital signs upon presentation were a blood pressure of 153/72 mmHg, a heart rate of 74 beats per minute, a respiratory rate of 20 breaths per minute, and a body temperature of 37.2°C. Physical examination showed a 0.5-cm penetrating wound in the left axilla, but no active bleeding was observed. The left lung sounds were slightly diminished, but no resonance or turbidity was observed (Fig. 1). On a chest X-ray, a radio-opaque foreign body was observed in the left lung field (Fig. 2), and chest computed tomography (CT) revealed infiltration of the lung parenchyma in the direction of the aortic arch from the left side, and a foreign body suspected to be a bullet near the aortic arch was noted. No hemothorax or pneumothorax was observed (Fig. 3). Exploratory video-assisted thoracotomy was attempted, but extensive pleural adhesion was observed; therefore, the operation was converted to open thoracotomy due to an inability to enter through the pleural adhesion. The left upper lobe was dissected carefully using a sponge stick, a peanut sponge, and electrocautery, and the entrance wound was observed in the lateral aspect of the left upper lobe (Fig. 4). As the pellet was not palpated, the location was confirmed using a C-arm (Fig. 5), and the pellet was removed by direct incision into the parenchyma (Fig. 6). The injured lung was closed using a single running locked suture and a continuous over-and-over suture. The bullet entrance was observed without sealing because no air leakage was observed; only a hemorrhagic contusion was visible and no other damage was detected.
CASE REPORT
- Injuries caused by GSWs are characterized by direct damage from bullets and burns, and incidental explosive effects. Patients should receive prompt initial management and rapid evacuation to a trauma center. GSWs are classified into low-velocity GSWs, including most handguns with firing speeds of less than 350 m/s; intermediate-velocity GSWs, including shotguns with firing speeds of 350–500 m/s; and high-velocity GSWs from military and hunting rifles with firing speeds above 600 m/s. Usually, a faster bullet results in a higher risk of injury or wound contamination. However, the degree of damage decreases with the distance of launch, and local wounds are not always accompanied by an internal injury due to bone involvement or abdominal penetration [6]. High-velocity bullets cause excessive damage to the surrounding tissues and are characterized by larger exit holes than entry holes, while low-velocity bullets, such as in this case, mainly create through-windows in tissues and have less destructive force than high-speed bullets. The inlet is relatively clear and there is often no outlet. These wounds also have the property of causing tissue damage due to large numbers of fragments with low-speed propagation paths [7,8]. In this case, neither hemothorax nor pneumothorax were present due to the severe adhesion of the pleura.
- A medical history and X-ray examination are essential for the diagnosis of foreign bodies. If the foreign body is metal, simple X-rays are most useful. CT can also be helpful for identifying the exact location and trajectory of the bullet. However, radial artifacts appearing around large metal objects often interfere with the adjacent structures on CT. In this case, we could easily identify the metallic foreign body on the chest X-ray at the first visit. X-ray fluoroscopy is also effective for removing foreign bodies stuck to the tissue during surgery.
- A shotgun wound can be treated with care, antibiotics, and tetanus vaccination. If the bullet remains in the lung parenchyma, conservative treatment may be performed rather than surgery for stable patients, but it is not yet an established treatment method. Delayed complications have been reported in rare cases when the bullet was not removed from the chest wound [1-5]. Conservative treatment may not be adequate due to a risk of complications such as major vascular embolism, progression, and migration to blood vessels. In the early stages, it may be possible to remove the foreign body through a simple incision. However, because of the above-mentioned complications, pulmonary resection may be necessary.
- The main component of a typical bullet is lead. Lead poisoning from gunshot wounds is unusual. but the complications of lead poisoning are serious. There has long been controversy regarding recommendations regarding early thoracotomy in patients with gunshot injuries [9-11]. In the face of the possibility of embolization or migration of the bullet or pellets or infection or fibrosis arising from foreign material within the thoracic cavity, it is always better to explore the wound before complications occur [12].
DISCUSSION
Fig. 3.(A) Infiltration running along the projectile path from the left chest wall to the interior. (B) A foreign body was observed near the aortic arch.
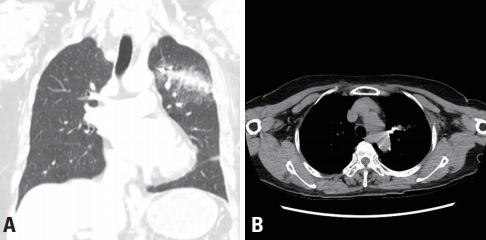

Fig. 4.Intraoperative findings on the left side. Entrance wounds were observed in the lateral aspect of the upper lung.


Fig. 5.Intraoperative C-arm imaging. DeBakey forceps were used to indicate the position of the foreign body in the upper lung field.


- 1. Kelley WA, James EC. Retained intrapulmonary bullet presenting with bronchial obstruction. J Trauma 1976;16:153–4. ArticlePubMed
- 2. Saunders MS, Cropp AJ, Awad M. Spontaneous endobronchial erosion and expectoration of a retained intrathoracic bullet: case report. J Trauma 1992;33:909–11. ArticlePubMed
- 3. Panichabhongse V, Kasantikul V, Panichabhongse S, Kanluan S. Bullet embolus to the right pulmonary artery after abdominal gunshot wound with “piggyback bullet”. J Med Assoc Thai 1996;79:676–9. PubMed
- 4. Symbas PN, Harlaftis N. Bullet emboli in the pulmonary and systemic arteries. Ann Surg 1977;185:318–20. ArticlePubMedPMC
- 5. Sherlock DJ, Jones B, Williams CR. Bullet wounds of the left lower chest and arterial bullet embolism. J R Coll Surg Edinb 1984;29:214–7. PubMed
- 6. Stefanopoulos PK, Hadjigeorgiou GF, Filippakis K, Gyftokostas D. Gunshot wounds: a review of ballistics related to penetrating trauma. J Acute Dis 2014;3:178–85. Article
- 7. Gant TD, Epstein LI. Low-velocity gunshot wounds to the maxillofacial complex. J Trauma 1979;19:674–7. ArticlePubMed
- 8. Berlin R, Gelin LE, Janzon B, Lewis DH, Rybeck B, Sandegård J, et al. Local effects of assault rifle bullets in live tissues. Acta Chir Scand Suppl 1976;459:1–76. PubMed
- 9. Meggs WJ, Gerr F, Aly MH, Kierena T, Roberts DL, Shih R, et al. The treatment of lead poisoning from gunshot wounds with succimer (DMSA). J Toxicol Clin Toxicol 1994;32:377–85. ArticlePubMed
- 10. Ellenhorn MJ. Metals and related compounds. In: Seth N. Schonwald, Ordog G, Wasserberger J, eds. Ellenhorn’s medical toxicology: diagnosis and treatment of human poisoning. 2nd ed. London:Elsevier;1997:1563-79.
- 11. Gerami S, Cousar JE 3rd, Davie JM, Moseley TM. The management of gunshot wounds of the chest. Ann Thorac Surg 1968;5:189–92. Article
- 12. Tanmoy G, Sandeep Kumar K, Chaitali S, Chiranjib B, Manasij M. Thoracic gunshot wound: a report of 3 cases and review of management. J Univer Surg 2015;3:1–5.
REFERENCES
Figure & Data
References
Citations
Citations to this article as recorded by 

 KST
KST



 PubReader
PubReader ePub Link
ePub Link Cite
Cite