Articles
- Page Path
- HOME > J Trauma Inj > Volume 31(2); 2018 > Article
-
Case Report
Endovascular Salvage for Traumatic Midthoracic Aortic Rupture with Left Diaphragmatic Injury - Shin-Ah Son, M.D.1, Tak-Hyuk Oh, M.D.1, Gun-Jik Kim, M.D.2, Deok Heon Lee, M.D., Ph.D.2, Kyoung Hoon Lim, M.D.3
-
Journal of Trauma and Injury 2018;31(2):66-71.
DOI: https://doi.org/10.20408/jti.2018.31.2.66
Published online: August 31, 2018
- 3,072 Views
- 24 Download
1Department of Thoracic and Cardiovascular Surgery, Kyungpook National University Hospital, Daegu, Korea
2Department of Thoracic and Cardiovascular Surgery, School of Medicine, Kyungpook National University, Kyungpook National University Hospital, Daegu, Korea
3Department of Surgery, School of Medicine, Kyungpook National University, Kyungpook National University Hospital, Daegu, Korea
- Correspondence to Kyoung Hoon Lim, M.D., Department of Surgery, Kyungpook, National University Hospital, 130 Dongdeok-ro, Jung-gu, Daegu 41944, Korea, Tel: +82-53-200-5605, Fax: +82-53-420-0510, E-mail: drlimkh@knu.ac.kr
• Received: May 31, 2018 • Revised: July 2, 2018 • Accepted: July 4, 2018
Copyright © 2018 The Korean Society of Trauma
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
- Patients with traumatic aortic rupture rarely reach the hospital alive. Even among those who arrive at the hospital alive, traumatic aortic rupture after high-speed motor vehicle accidents leads to a high in-hospital mortality rate and is associated with other major injuries. Here, we report a rare case of descending midthoracic aortic rupture with blunt diaphragmatic rupture. Successful management with emergency laparotomy after an immediate endovascular procedure resulted in a favorable prognosis in this case.
- The incidence of traumatic aortic injury (TAI) secondary to blunt trauma due to high-speed transportation accidents is rapidly increasing. TAI in accident survivors undoubtedly represents a direct threat to life and requires a fast-track diagnostic and therapeutic plan for a successful resuscitation.
INTRODUCTION
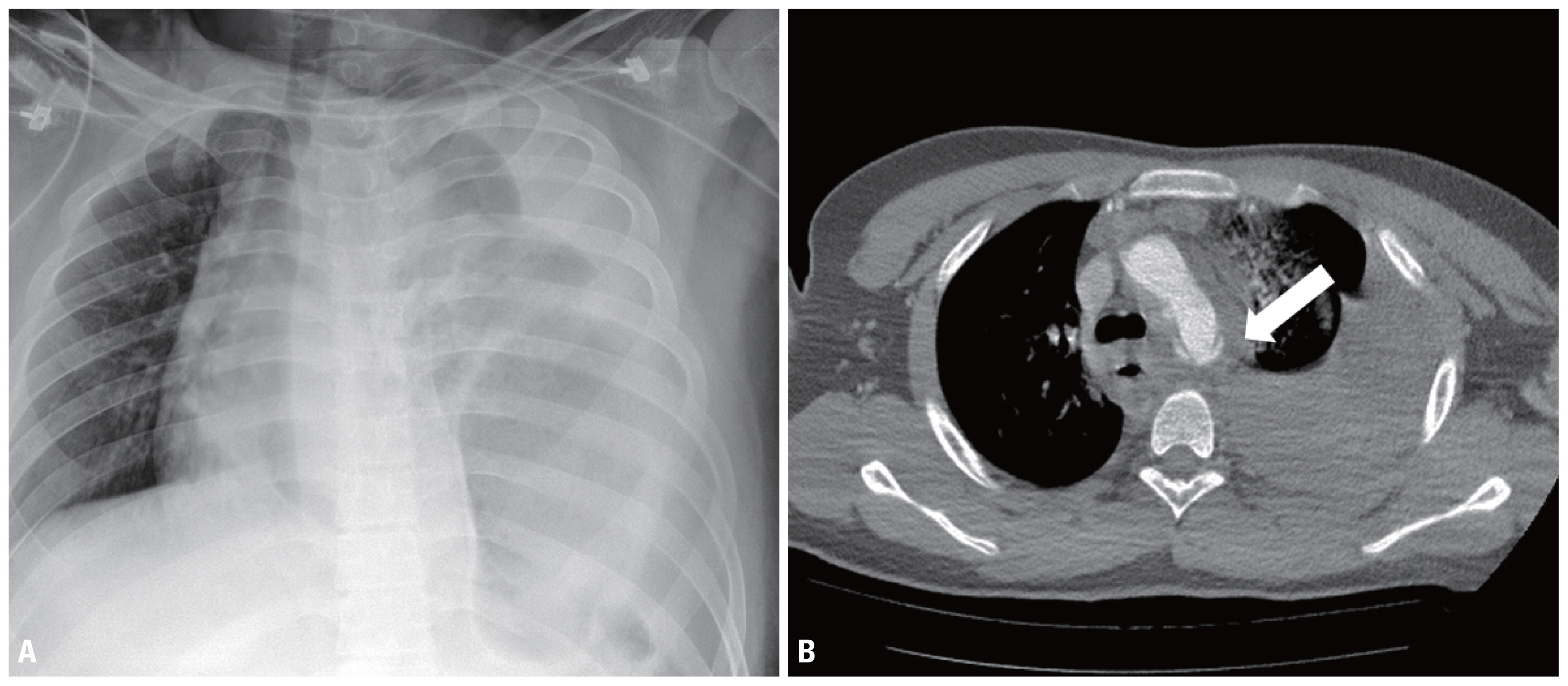
- A 19-year-old man with no prior medical history was struck by a motor vehicle while riding his motorcycle, and was admitted to our trauma center with 119 emergency crews 10 minutes after the accident. His initial systolic blood pressure and heart rate were 180 mmHg and 136 beats/minute, respectively, and he was mentally alert. However, he shortly became hemodynamically unstable and developed a drowsy mental status. He required mechanical ventilator support and was intubated. Moreover, simultaneous initial investigations were conducted with computed tomography (CT) and focused assessment with sonography for trauma (FAST). Initial chest CT showed aortic isthmus rupture with a large amount of hematoma around the aorta and left hemothorax (Fig. 1), and descending mid thoracic aortic rupture with stomach herniation (Fig. 2).
- The trauma team immediately decided to perform emergency thoracic endovascular aortic repair first, followed by exploratory laparotomy. Before entering the operating room, the patient’s vital sign was 80/40 mmHg with a low dose of inotropes. In the operating room, we tried to maintain his systolic blood pressure to about 70–80 mmHg to prevent aortic rupture aggravation. Under general anesthesia, the aortic rupture was excluded using two S&G SEAL thoracic stent grafts (24×20×110 mm and 24×24×110 mm; S&G Biotech, Seongnam, Korea). There were no complications during the procedure, and oversizing of the stent grafts relative to the aorta did not exceed 10% to provide adequate radial force to keep the deployed stent grafts in place. Post-deployment aortography showed laminar blood flow through the devices and the thoracic aorta with complete exclusion of the two injured aortic segments. After routine closure, exploratory laparotomy was performed.
- Under the upper midline incision, all abdominal organs were found intact, with no signs of intra-abdominal bleeding. A large radial defect (nearly 10 cm) was detected, and the stomach and spleen were herniated. The ruptured diaphragmatic rims were sutured using 2-0 prolene; a chest tube was inserted into the left thoracic cavity; and the surgery was completed. The total operative time was 185 minutes, and the total contrast agent amount was 120 mL.
- The patient was moved to the trauma intensive care unit (TICU). The postoperative vital signs were unstable with high doses of vasopressor and inotropes; however, neurological adverse events such as paraplegia were not found. The patient’s postoperative laboratory findings were glutamic-oxaloacetic acid transaminase/glutamic-pyruvic acid transaminase 4,600/2,700 IU/L, blood urea nitrogen/creatinine 38/2.7 mg/dL, and pH 7.2, and these were compatible findings of overall organ ischemia. The TICU team helped the patient with fast and successful resuscitation, and his condition gradually improved after hemodialysis and hydration. He was extubated on postoperative day (POD) 5. His vital signs and condition were good, despite the presence of persistent fever.
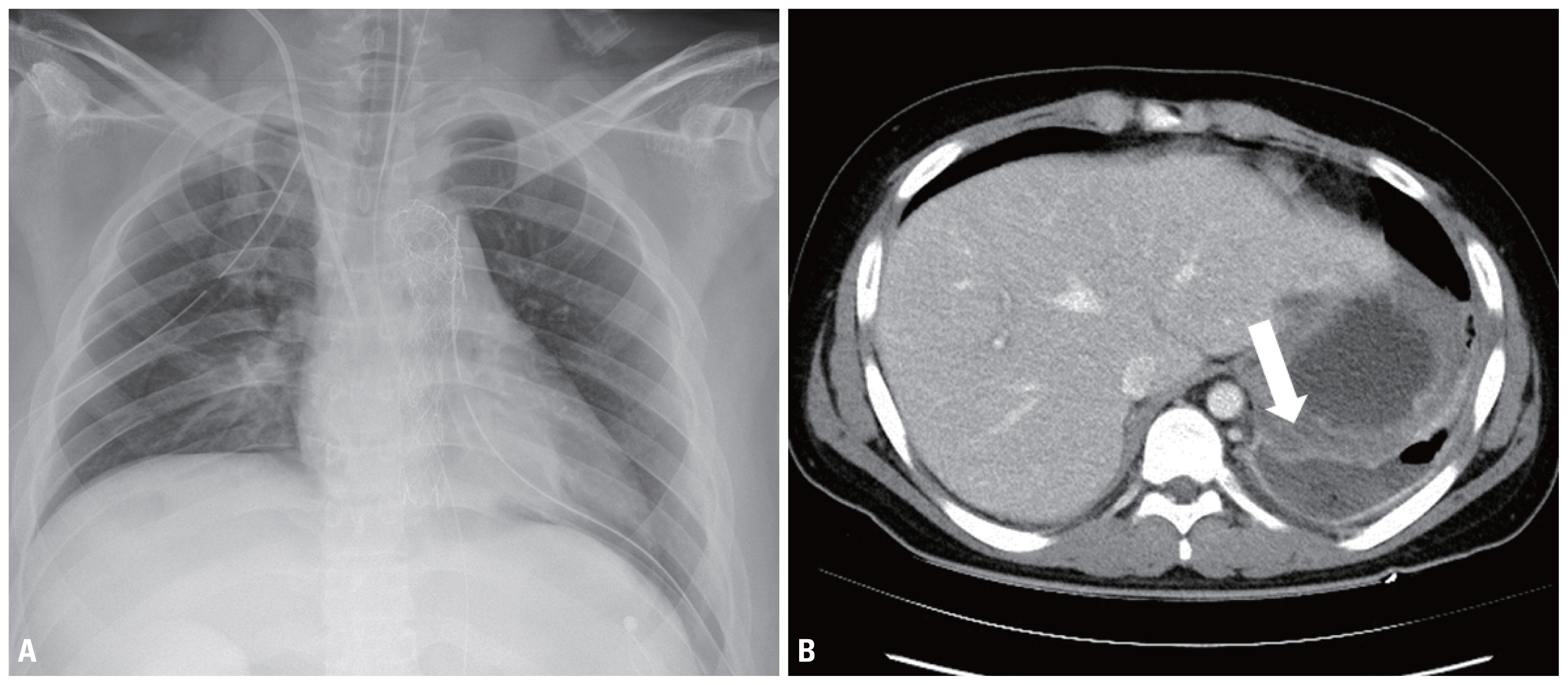
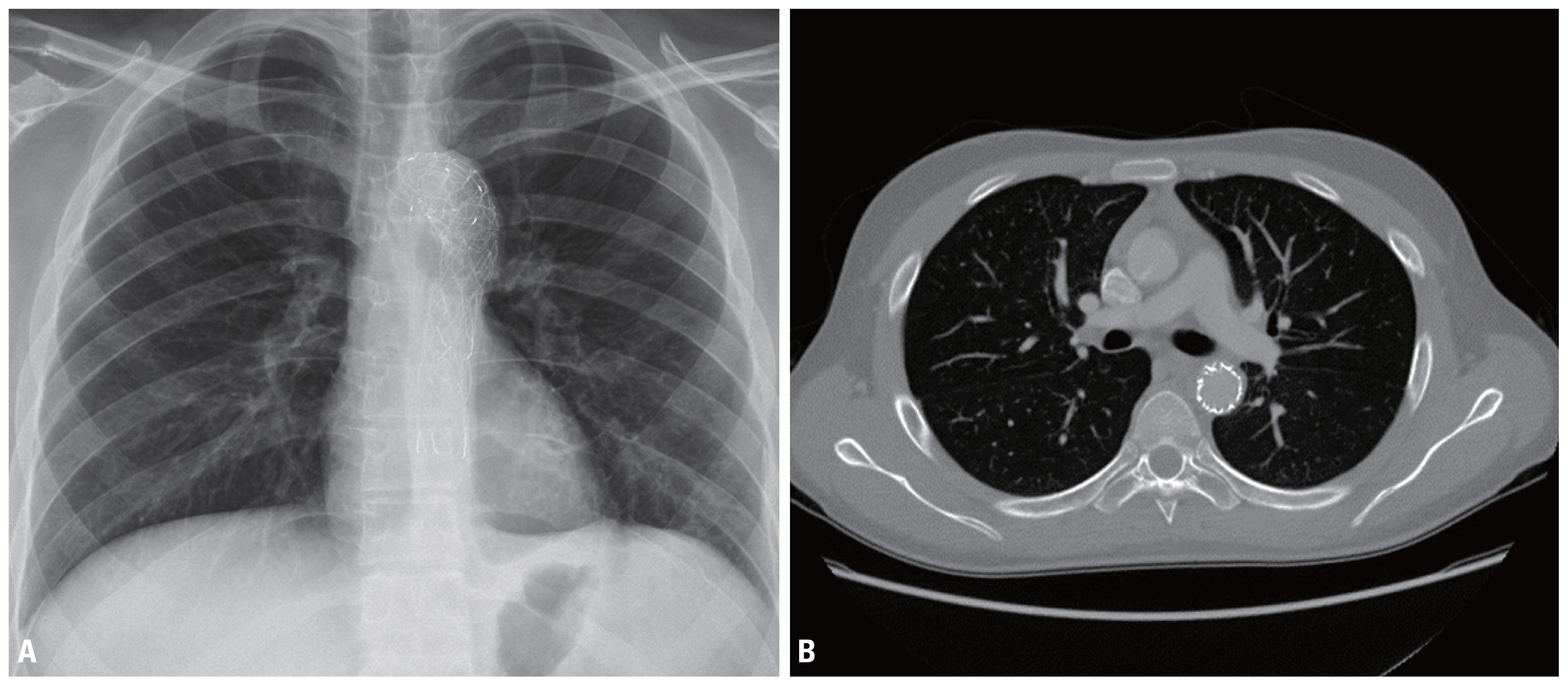
- After POD 17, follow-up abdominal CT showed gallbladder and gastric fundus necrosis (Fig. 3). The gastric fundus was partially resected, and cholecystectomy was performed. His fever was controlled and his general condition improved after a second exploratory laparotomy. With stable vital signs, he underwent open reduction and internal fixation for distal radial fractures on POD 30 and was discharged on POD 45 without complications (Fig. 4).
CASE REPORT
- TAI occurs in 2% of patients with blunt thoracic trauma and is often considered a life-threatening injury [1]. It was historically estimated that prehospital mortality occurred in >75% of patients, and up to 50% of those arriving at the hospital alive died within the first 24 hours after injury [2].
- TAI mostly occurs at sites of aortic tethering, such as the aortic root, isthmus, and diaphragmatic hiatus. Injuries at the isthmus and abdominal aorta are the most commonly observed injuries during surgery [3]. Teixeira et al. [4] recently reported on fatal blunt trauma in 104 victims. The most common site of traumatic thoracic aortic injury was the isthmus and the descending aorta, occurring in 67 fatalities (66% of patients with traumatic thoracic aortic injuries). When classified with respect to the descending aorta (proximal descending thoracic aorta [2 cm below the ostium of the left subclavian artery], midthoracic aorta [at the level of the left inferior pulmonary vein]), TAI occurs in the proximal descending thoracic aorta in the vast majority of cases [5].
- Patients with TAI were significantly more likely to have other associated injuries. Rizoli et al. [6] reported the following associated injuries: cardiac injury (44%), hemothorax (86%), rib fractures (86%), and intra-abdominal injury (74%). In this case, the incidence rate of blunt diaphragmatic rupture (BDR) associated with TAI ranged from 5.9% to 16%.
- CT and FAST are the image modalities of choice in patients with multiorgan trauma at the emergency department. However, CT angiography (CTA) has the highest diagnostic sensitivity for TAI. CTA has a diagnostic sensitivity of 98% and a diagnostic specificity of nearly 100% for TAI. The definitive signs of TAI are active contrast extravasation, rupture, intramural hematoma, and dissection [7]. Chest radiography is vital in diagnosing BDR and is repeatedly referred to as the single most accurate screening test.
- Two different pathophysiologic mechanisms of TAI are believed to play a role in victims of frontal collisions. First, a shearing injury to the aorta can occur because of the differential deceleration rate of the heart and aortic arch relative to its point of fixation. Second, stress forces can occur at the ligamentum arteriosum, as the aorta is distorted by compression against the vertebral column [8]. This mechanism generally occurs at the aortic isthmus. In this case, aortic rupture in two segments, the aortic isthmus and the descending midthoracic aorta, is uncommon.
- TAIs are classified according to their severity. According to Azizzadeh et al. [9], aortic injuries can be categorized into type I (intimal tear), type II (intramural hematoma), type III (pseudoaneurysm), or type IV (rupture). Pseudo-aneurysms are present in about 70% of TAIs, and 90% of TAIs occur at the isthmus. However, type IV injuries have a high mortality rate because of several other severe associated injuries, high Injury Severity Score, and unstable vital signs at the emergency department [10].
- The only treatments for type III–IV injuries before the era of endovascular procedures were extensive classical surgical procedures such as the clamp-and-sew technique and the bypass technique, which have high mortality rates ranging between 15% and 45% [11]. The conventional surgical repair is associated with a marked blood pressure decrease in patients and a significantly longer surgical time. These factors contribute to more frequent postoperative cardiopulmonary failure and neurological adverse events such as paraplegia. The overall mortality rate after surgical descending aortic procedures is much higher than that after endovascular procedures [11,12].
- Endovascular techniques for the treatment of TAI were first successfully performed in 1997 by Semba et al. [12]. Although endovascular techniques are generally recognized as an alternative to open surgery, there are common postoperative adverse events associated with endovascular devices, such as endoleaks, stent graft migration, retrograde type A aortic dissection, new-onset dissection, and distal redissection. The most dangerous clinical problem in the treatment of descending aortic pathologies is the high risk of ischemic spinal cord injury, which occurs in 21% of patients undergoing open surgery and 2–12% of patients treated with endovascular procedures [13].
- Traumatic descending aortic injury with BDR is occasionally reported. However, our case showing midthoracic aortic rupture with BDR is an extremely rare case with a high mortality risk. In this case, the injury posed a direct threat to the patient’s life, which required significant promptness in the diagnosis of aortic injury. Rapid transportation and a fast-track diagnostic and therapeutic plan for a successful resuscitation prevented a devastating injury that could have resulted in death. Moreover, the space-occupying effect of the herniated stomach due to the diaphragmatic rupture in the left thoracic cavity might have prevented the progression of hemothorax and aortic rupture. We believe that this effect conferred a hopeful outcome for the patient. Moreover, the patient developed persistent postoperative fever, which delayed his healing. We suspected that his fever was induced by the necrosis of the injured diaphragmatic tissue caused by the ischemic change due to low blood pressure. In the second operation, we found that the previous diaphragmatic sutures were all dissolved and nearby organs such as the gallbladder and gastric fundus also showed necrotic change. Eventually, postoperative organ ischemia was believed to have delayed the patient’s healing.
- In conclusion, TAI is one of the most devastating injuries related to high-speed vehicular accidents that trauma surgeons encounter. We reported on successful management of a midthoracic aortic rupture with BDR, a very rare case compared with other trauma injuries, which was achieved through the rapid coordination of all involved specialties and led to a favorable prognosis.
DISCUSSION
ACKNOWLEDGMENTS
Fig. 1Initial chest X-ray and chest CT. Chest X-ray show stomach herniation and large amount of hemothorax (A). And chest CT show aorta isthmus rupture (arrow) with large amount of hematoma around aorta and left hemothorax (B). CT: computed tomography.


Fig. 2(A, B) Initial chest CT (other view). Chest CT show descending mid thoracic aorta rupture (arrows) with hematoma apart from isthmus and left diaphragmatic rupture accompanied stomach herniation. CT: computed tomography.


Fig. 3(A, B) Postoperative chest X-ray and chest CT. Chest X-ray show endovascular stent graft in descending aorta and well-repaired diaphragm (A). In the performed chest CT due to the patient’s persistent fever on POD 17, communication of left diaphragm and stomach (arrow) was suspected and air fluid collection in left pleural cavity was showed (B). The patient underwent exploratory laparotomy, GB necrosis and gastric fundus necrosis were caused the patient’s fever. CT: computed tomography, POD: postoperative day, GB: gallbladder.
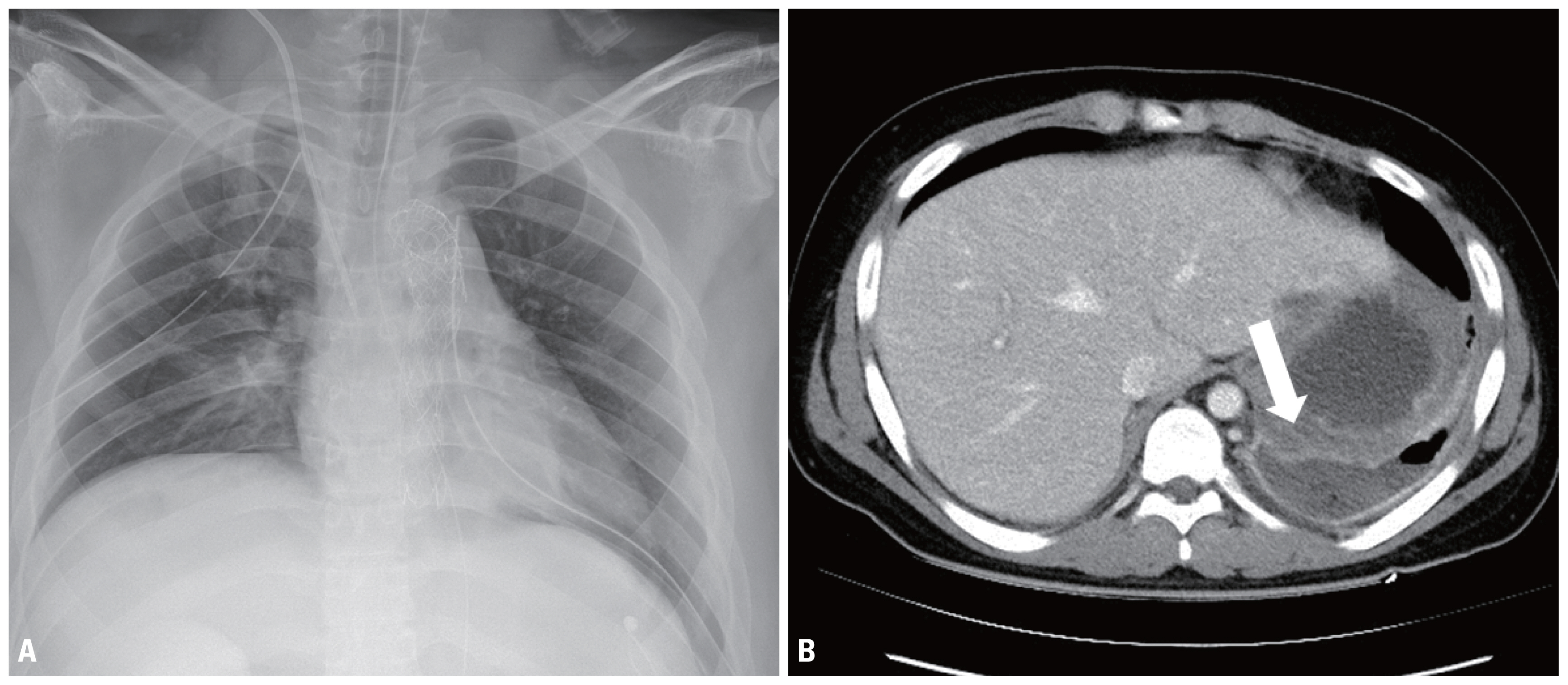

Fig. 4(A, B) Following chest X-ray and chest CT before hospital discharge. Endovascular stent graft in descending aorta was well functioned and no evidence of endoleak. The patient discharged on POD 45 without complications. CT: computed tomography, POD: postoperative day.


- 1. Ungar TC, Wolf SJ, Haukoos JS, Dyer DS, Moore EE. Derivation of a clinical decision rule to exclude thoracic aortic imaging in patients with blunt chest trauma after motor vehicle collisions. J Trauma 2006;61:1150–5.ArticlePubMed
- 2. Fabian TC, Richardson JD, Croce MA, Smith JS Jr, Rodman G Jr, Kearney PA, et al. Prospective study of blunt aortic injury: Multicenter Trial of the American Association for the Surgery of Trauma. J Trauma 1997;42:374–80; discussion 380–3, ArticlePubMed
- 3. Williams JS, Graff JA, Uku JM, Steinig JP. Aortic injury in vehicular trauma. Ann Thorac Surg 1994;57:726–30.ArticlePubMed
- 4. Teixeira PG, Inaba K, Barmparas G, Georgiou C, Toms C, Noguchi TT, et al. Blunt thoracic aortic injuries: an autopsy study. J Trauma 2011;70:197–202.ArticlePubMed
- 5. Faure EM, Canaud L, Agostini C, Shaub R, Böge G, Marty-ané C, et al. Reintervention after thoracic endovascular aortic repair of complicated aortic dissection. J Vasc Surg 2014;59:327–33.ArticlePubMed
- 6. Rizoli SB, Brenneman FD, Boulanger BR, Maggisano R. Blunt diaphragmatic and thoracic aortic rupture: an emerging injury complex. Ann Thorac Surg 1994;58:1404–8.ArticlePubMed
- 7. Nagpal P, Mullan BF, Sen I, Saboo SS, Khandelwal A. Advances in imaging and management trends of traumatic aortic injuries. Cardiovasc Intervent Radiol 2017;40:643–54.ArticlePubMedPDF
- 8. van Leeuwen JE, Broos PL, Rommens PM, Nevelsteen A. Combined blunt rupture of the diaphragm and thoracic aorta. Injury 1990;21:117–9.ArticlePubMed
- 9. Azizzadeh A, Keyhani K, Miller CC 3rd, Coogan SM, Safi HJ, Estrera AL. Blunt traumatic aortic injury: initial experience with endovascular repair. J Vasc Surg 2009;49:1403–8.ArticlePubMed
- 10. Starnes BW, Lundgren RS, Gunn M, Quade S, Hatsukami TS, Tran NT, et al. A new classification scheme for treating blunt aortic injury. J Vasc Surg 2012;55:47–54.ArticlePubMed
- 11. von Oppell UO, Dunne TT, De Groot MK, Zilla P. Traumatic aortic rupture: twenty-year metaanalysis of mortality and risk of paraplegia. Ann Thorac Surg 1994;58:585–93.ArticlePubMed
- 12. Semba CP, Kato N, Kee ST, Lee GK, Mitchell RS, Miller DC, et al. Acute rupture of the descending thoracic aorta: repair with use of endovascular stent-grafts. J Vasc Interv Radiol 1997;8:337–42.ArticlePubMed
- 13. Setacci F, Sirignano P, De Donato G, Chisci E, Galzerano G, Massaroni R, et al. Endovascular thoracic aortic repair and risk of spinal cord ischemia: the role of previous or concomitant treatment for aortic aneurysm. J Cardiovasc Surg (Torino) 2010;51:169–76.PubMed
REFERENCES
Figure & Data
References
Citations
Citations to this article as recorded by 

 KST
KST

 PubReader
PubReader ePub Link
ePub Link Cite
Cite