Articles
- Page Path
- HOME > J Trauma Inj > Volume 36(1); 2023 > Article
-
Case Report
Successful surgical intervention in traumatic carotid artery thrombosis after a motor vehicle accident: a case report -
Görkem Yiğit, MD

-
DOI: https://doi.org/10.20408/jti.2021.0095
Published online: June 29, 2022
- 1,797 Views
- 64 Download
Department of Cardiovascular Surgery, Yozgat City Hospital, Yozgat, Turkey
- Correspondence to Görkem Yiğit, MD Department of Cardiovascular Surgery, Yozgat City Hospital, Erdoğan Akdağ Mah, Viyana Cad., Yozgat 66100, Turkey Tel: +90-506-677-75-77 Email: drgorkemyigit@gmail.com
• Received: November 16, 2021 • Revised: December 10, 2021 • Accepted: December 16, 2021
Copyright © 2022 The Korean Society of Traumatology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
- Blunt carotid artery injury can lead to impaired brain perfusion due to ischemic stroke and thromboembolic events. To reduce the risk of potential neurological complications, it is critical to determine the diagnosis and management protocol as quickly as possible after a detailed clinical examination. This report presents successful surgical treatment of a young male patient who developed a traumatic left common carotid artery thrombosis after a motor vehicle accident.
- Motor vehicle accidents are the most common cause of blunt carotid artery injuries (BCAIs) [1]. Carotid artery injury can result in dissection, an intramural thrombus, or pseudoaneurysm, leading to decreased blood flow to the brain and thromboembolic events [2]. Moreover, BCAIs cause delayed neurological injuries, with an estimated mortality risk of 40% and irreversible neurological disorders in more than 10% of cases [3,4]. Early diagnosis and prompt management of BCAIs could dramatically reduce the incidence of thromboembolic events [5]. This report presents the successful surgical treatment of a young male patient who developed a traumatic left common carotid artery thrombosis after a motor vehicle accident.
INTRODUCTION
- Following a motor vehicle accident, a previously healthy 19-year-old male patient was admitted to the emergency department (ED). On admission, he had stable vital signs, normal mental ability, speech, and cranial nerve examination findings, as well as a Glasgow Coma Scale score of 15. However, he had paresthesia in his right-hand fingertips with no motor dysfunction, and normal sensory and motor examination findings on other extremities. There were also no remarkable findings in other systems. Initial laboratory tests and radiography of the skull, spine, chest, and serial extended focused assessment with sonography for trauma were normal. Finally, no other traumatic lesions were reported. Due to paresthesia in the fingertips, cranial, cervical, and lumbar spine computed tomography and magnetic resonance imaging examinations were performed as part of the simultaneous evaluation by a neurosurgeon. No neurological pathology requiring surgical intervention was encountered.
- The patient was also evaluated using craniocervical and thoracic computed tomography angiography (CTA) with the suspicion of vascular trauma. The patient's cranial CTA scans revealed a completely normal blood supply to the brain without any signs of hypoperfusion. Cervical CTA showed that the left common carotid artery (CCA) after the first 6-cm segment was totally occluded due to thrombosis (Fig. 1). Subsequently, no flow was observed until the carotid bifurcation (Fig. 1B). The left internal carotid artery and external carotid artery were observed to be patent (Fig. 1C). It was thought that reverse flow occurred in the external carotid artery branches, and consequently, the external carotid artery filled the internal carotid artery retrogradely. An intravenous bolus of heparin (80 IU/kg) was administered immediately, and emergency surgery was decided. Following general anesthesia, the left-sided CCA and its bifurcation were exposed without touching the vessels using standard exposure. Although no shunt was used, hypertension was managed to improve contralateral cerebral perfusion. After longitudinal arteriotomy, there was clearly a 1 × 0.5-cm thrombus without a dissection flap at the level of the left CCA. The organized thrombus material was removed and the simple laceration in the intima was repaired primarily. No other pathology was observed within the lumen of the artery. By removing the clamps, good retrograde and antegrade flows were observed. Metronidazole, ceftriaxone, and low-molecular-weight heparin were started as medications in the intensive care unit. Furthermore, after 3 days, the low-molecular-weight heparin was switched to oral warfarin to ensure long-term thromboembolism prevention. In the postoperative phase, no neurological or hemodynamic problems were observed. The radiologist confirmed that the flow velocities were within normal values during a carotid Doppler ultrasonography (CDUSG) examination. On the 7th postoperative day, the patient was discharged with warfarin therapy without any hemorrhagic complications. A neurological examination after 1 month revealed completely normal motor function and sensations in the extremities, without any other surgical complications. Neither residual stenosis of the left CCA, nor progression of the stenosis of the CCA was documented on carotid CTA (Fig. 2). There was no residual stenosis in the results of carotid CDUSG at the 6-month follow-up. Written informed consent for publication of the research details and clinical images was obtained from the patient.
CASE REPORT
- Vessel stretching can cause intimal damage, which can lead to dissection or intramural thrombus formation, resulting in stenosis or total occlusion after blunt trauma to the neck [5–7]. Moreover, these pathologies lead to impaired brain perfusion due to ischemic stroke and thromboembolic events. Although more than half of BCAI patients may be asymptomatic at the first visit to the ED, delayed neurological complications may occur from 1 hour to 7 days after injury [8]. There was only mild paresthesia on the right-hand fingertips in this patient who was admitted to the ED with multiple trauma. The patient had no motor deficits. After a detailed physical examination without losing time, advanced diagnostic methods were applied to minimize the risk of a potential neurological complication.
- Fast and comprehensive screening of the head and neck arteries based on signs has been recommended for early diagnosis and treatment of BCAIs [9]. BCAIs are diagnosed by four imaging techniques: CDUSG, CTA, magnetic resonance angiography, and digital subtraction angiography. Although CTA has often been recommended as a diagnostic method in several reports, digital subtraction angiography remains the gold-standard diagnostic tool for neck artery injuries [5,9]. CDUSG, in contrast, is not widely used for assessing neck trauma and lacks sufficient sensitivity in identifying carotid artery injuries [10]. Since CDUSG is highly operator-dependent and requires experience, CTA was preferred as the primary diagnostic tool in this patient.
- BCAI treatment aims to slow the progression of the arterial injury, reduce the risk of ischemic events in asymptomatic cases, and improve the neurological and survival results [11]. Early antithrombotic or anticoagulant therapy was recommended for BCAI patients in previous studies [12]. However, these treatments may be contraindicated in patients who have coagulopathy or intracranial bleeding as a result of blunt multitrauma. Depending on imaging findings, Biffl et al. [13] described what have become the most widely accepted grading criteria for BCAIs. BCAIs can be categorized into five subtypes using this scale: (1) luminal irregularity or dissection with <25% stenosis; (2) dissection or intramural hematoma with ≥25% stenosis; (3) traumatic aneurysm; (4) occlusion; and (5) transection. The present case was classified as subtype IV. Especially, grade IV and grade V injuries are associated with increased morbidity and mortality rate, and survival is related to the severity of neurological injury at the time of diagnosis [14]. Surgical repair of accessible grade IV or grade V BCAIs is recommended by many authors in large cohort studies [9,15]. The patient's emergency operation was performed 2 hours after admission to the ED. Therefore, it was thought that an early surgical approach would be more appropriate because of total occlusion in the carotid artery and accompanying paresthesia in the extremity after imaging. It was thought that conservative treatment might lead to late neurological complications in this young patient. Primary repair of the simple intimal laceration, along with surgical thrombectomy, was thought to provide the maximal benefit to the patient. An excellent result was obtained in terms of symptomatic regression and survival.
- It should never be forgotten that trauma surgery is a crucial part of cardiovascular surgery. With the effective use of early diagnostic methods, performing open surgery instead of conservative treatment prevented a possible permanent neurological deficit in this young patient. However, despite previous cohort studies of the management of carotid trauma, prospective randomized clinical trials with large samples are needed to create more up-to-date treatment algorithms.
- In conclusion, BCAI is an uncommon but potentially lethal condition that requires immediate diagnosis and treatment. To reduce the risk of a potential neurological complication, it is critical to determine the diagnosis and management protocol as quickly as possible after a detailed clinical examination.
DISCUSSION
-
Ethical statements
Written informed consent for publication of the research details and clinical images was obtained from the patient.
-
Conflicts of interest
The author has no conflicts of interest to declare.
-
Funding
None.
ARTICLE INFORMATION
Fig. 1.
(A) Axial CTA of the neck demonstrating thrombosis and occlusion in the left common carotid artery (arrow). (B) Nonopacification was seen at the left internal and external carotid artery bifurcation level (arrow). (C) The left internal carotid artery and external carotid artery showed patency at the level of the C2 vertebra (arrow). (D) Three-dimensional CTA examination of the carotid artery revealing total occlusion before the bifurcation level (arrow).
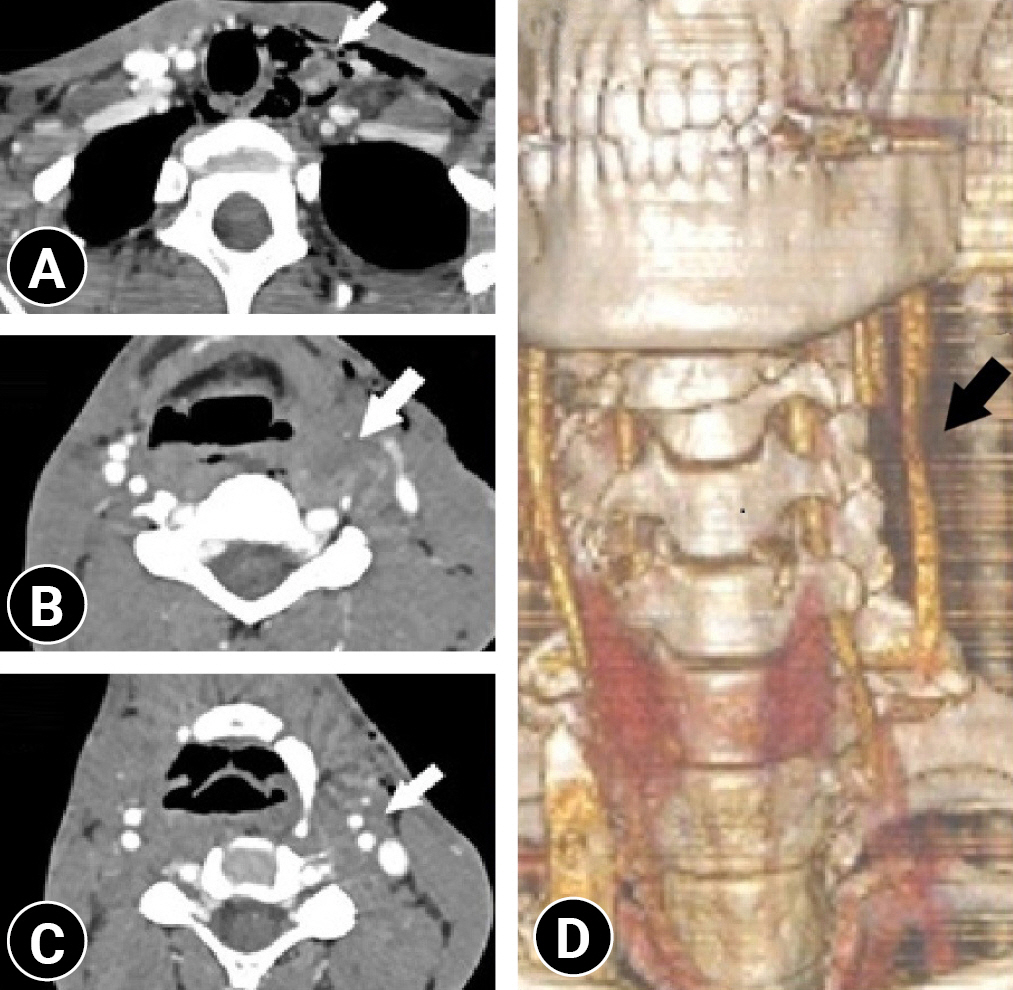
Initial cervical computed tomography angiography (CTA) scan of the axial and three-dimensional sections.

Fig. 2.
(A) Axial CTA of the neck demonstrating the normally contrasted left internal and external carotid arteries (arrow). (B, C) Normally contrasted left common carotid artery (arrows). (D) Sagittal CTA of the neck demonstrating the normally contrasted left common carotid artery (arrow). (E) Three-dimensional CTA examination of the carotid artery revealing no occlusion and completely normal blood flow (arrow).
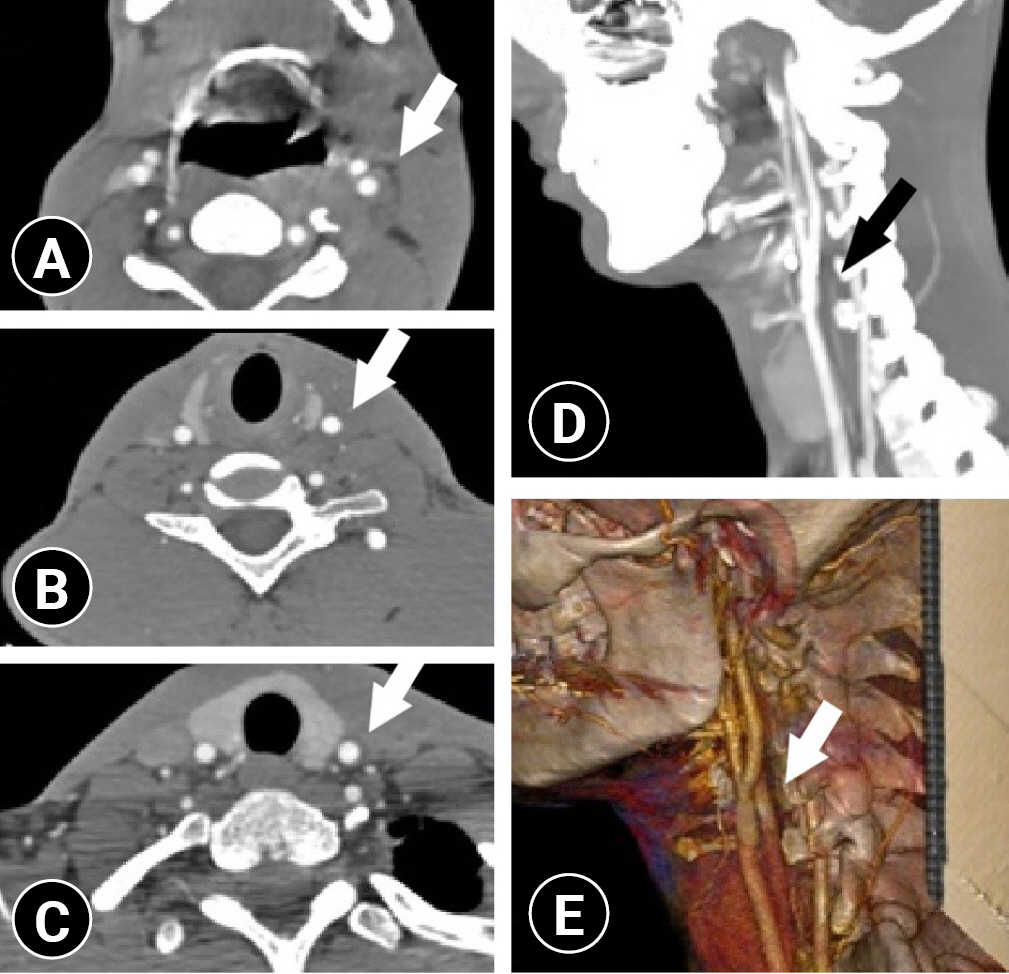
Postoperative cervical computed tomography angiography (CTA) scan of the axial and three-dimensional sections.

- 1. Srivastava A, Bradley M, Kelly M. Bilateral carotid artery dissection after high impact road traffic accident. J Radiol Case Rep 2008;2:23–8. ArticlePubMedPMC
- 2. Faridaalaee G, Naghipour B, Ahmadi S, Rahmani SH. Carotid artery thrombosis and cerebral infarction after multiple traumas. J Emerg Pract Trauma 2017;3:68–70. Article
- 3. Nagpal P, Policeni BA, Bathla G, Khandelwal A, Derdeyn C, Skeete D. Blunt cerebrovascular injuries: advances in screening, imaging, and management trends. AJNR Am J Neuroradiol 2017;39:406–14. ArticlePubMedPMC
- 4. Shafafy R, Suresh S, Afolayan JO, Vaccaro AR, Panchmatia JR. Blunt vertebral vascular injury in trauma patients: ATLS recommendations and review of current evidence. J Spine Surg 2017;3:217–25. ArticlePubMedPMC
- 5. Lee TS, Ducic Y, Gordin E, Stroman D. Management of carotid artery trauma. Craniomaxillofac Trauma Reconstr 2014;7:175–89. ArticlePubMedPMCPDF
- 6. Stein DM, Boswell S, Sliker CW, Lui FY, Scalea TM. Blunt cerebrovascular injuries: does treatment always matter? J Trauma 2009;66:132–44. ArticlePubMed
- 7. McKevitt EC, Kirkpatrick AW, Vertesi L, Granger R, Simons RK. Blunt vascular neck injuries: diagnosis and outcomes of extracranial vessel injury. J Trauma 2002;53:472–6. ArticlePubMed
- 8. Burlew CC, Biffl WL, Moore EE, Barnett CC, Johnson JL, Bensard DD. Blunt cerebrovascular injuries: redefining screening criteria in the era of noninvasive diagnosis. J Trauma Acute Care Surg 2012;72:330–7. ArticlePubMed
- 9. Biffl WL, Cothren CC, Moore EE, et al. Western Trauma Association critical decisions in trauma: screening for and treatment of blunt cerebrovascular injuries. J Trauma 2009;67:1150–3. ArticlePubMed
- 10. Khodayar M, Sotoodehnia M, Noyani A, Sheidaie H, Yekesadat S. The carotid artery thrombosis following blunt neck trauma; a case report. Front Emerg Med 2020;4:e94.
- 11. Li W, D’Ayala M, Hirshberg A, Briggs W, Wise L, Tortolani A. Comparison of conservative and operative treatment for blunt carotid injuries: analysis of the National Trauma Data Bank. J Vasc Surg 2010;51:593–9. ArticlePubMed
- 12. Blitzer DN, Ottochian M, O’Connor JV, et al. Timing of intervention may influence outcomes in blunt injury to the carotid artery. J Vasc Surg 2020;71:1323–32. ArticlePubMed
- 13. Biffl WL, Moore EE, Offner PJ, Brega KE, Franciose RJ, Burch JM. Blunt carotid arterial injuries: implications of a new grading scale. J Trauma 1999;47:845–53. ArticlePubMed
- 14. Cogbill TH, Moore EE, Meissner M, et al. The spectrum of blunt injury to the carotid artery: a multicenter perspective. J Trauma 1994;37:473–9. ArticlePubMed
- 15. Bromberg WJ, Collier BC, Diebel LN, et al. Blunt cerebrovascular injury practice management guidelines: the Eastern Association for the Surgery of Trauma. J Trauma 2010;68:471–7. ArticlePubMed
REFERENCES
Figure & Data
References
Citations
Citations to this article as recorded by 

- Figure
- Related articles
-
- Radiological assessment and follow-up of a nonsurgically treated odontoid process fracture after a motor vehicle accident in Egypt: a case report
- Portal vein embolization in intrahepatic portal vein injury after blunt trauma: a case report
- Successful management of a common carotid artery injury using a Pruitt-F3 Carotid Shunt: a case report
 KST
KST

 PubReader
PubReader ePub Link
ePub Link Cite
Cite



